Irreversible electroporation: A safe and effective therapy for low to intermediary prostate cancer risk profiles
Prostate cancer affects millions of men globally, and is also the third-largest cause of cancer-related deaths among men. Irreversible electroporation (IRE) is one of the more targeted, focal, and minimally aggressive therapies for prostate cancer ablation in comparison to radiotherapy, thermal, or cryo-based ablation methods. Distinguished scientist Professor Olivier Cussenot, surgeon urologist expert for the French National Cancer Institute, is working extensively on making IRE an optimal and effective treatment choice for patients living with prostate cancer.
Prostate cancer is the second most-diagnosed cancer in men. It affects about 100–112 men out of every 100,000 men in Australia, New Zealand, North America, and Europe. While low-risk prostate cancers under constant surveillance require brachytherapy or other forms of focal therapy, high-risk prostate cancers are treated through surgery and radiotherapy, with or without androgen deprivation (a method to reduce testosterone levels in prostate cancer). Yet, they are not short of debilitating effects.

Most prostate cancers do not pose significant risks of progression for as many as fifteen years, thus having less aggressive but effective therapies to treat them locally is always desirable. However, prostate cancer affects millions of men globally, and is also the third-largest cause of cancer-related deaths among men. This makes it important to find ways to treat prostate cancer in its early stages and prioritise patients’ quality of life and overall health, at the same time. Distinguished scientist Professor Olivier Cussenot, an expert for the French National Cancer Institute, advocates the use of irreversible electroporation (IRE) for patients living with prostate cancer.
What is irreversible electroporation?
Irreversible electroporation (IRE) refers to the application of targeted and controlled electric pulses to ablate (surgically remove) cancerous tissue using smart needles, with inbuilt electrodes and guided by imaging techniques. IRE can be delivered using the NanoKnife (Angiodynamics) or Dophi™ N3000 Electroporation System (Surgnova/HDTECH).
IRE is different from ablation processes needing heat, which are at risk of damaging other organs around the prostate gland, like the urethra, rectum, urinary bladder, sphincter muscle, and the surrounding cavernous nerves (a class of nerves responsible for penile erections) and tissue bundles. This gives IRE an advantage over other forms of aggressive therapies which pose a risk of developing urinary incontinence and erectile dysfunction, among others.
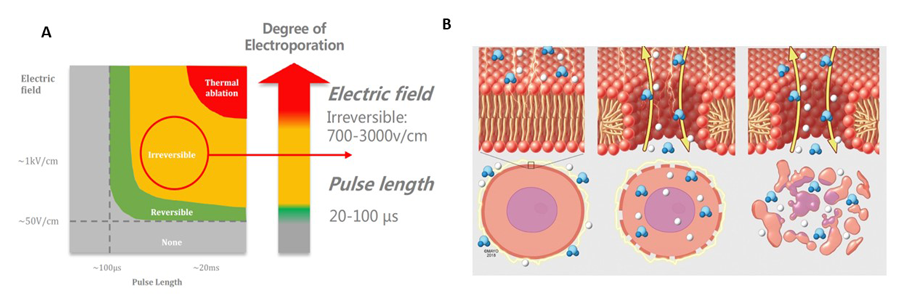
Firstly, the location of the cancerous tissue is determined using multiple prostate imaging modalities like high-quality magnetic resonance imaging (MRI), real-time ultrasound via a cognitive fusion or software-based MRI–US fusion system, transrectal ultrasound, prostate-specific membrane antigen (PSMA)-positron emission tomography (PET) scans; the location is then tallied with biopsy results. This positioning needs to be as accurate as possible for optimal benefits.
The number of electrodes placed also depends on the nature, size, and location of the tumour within the prostate. IRE uses an electric field with usually 90 pulses of 1,500 volts/cm delivered between pairs of electrodes. The application of electric current forms nanopores across the cancer tissue leading to apoptosis (cell death) and selective destruction of the cancerous tissue. IRE can also be applied to local, recurrent prostate cancer that has been previously exposed to radiotherapy or surgery, including when other partial ablation therapies have failed.
Optimal IRE application for patients
70% of all prostate cancers occur in the peripheral zone (outer part) of the prostate gland, followed by 25% of cases in the transitional zone (middle part), and the remaining 5% in the SMA (the inner most part – anterior fibromuscular stroma), due to the varying density of glands susceptible to transformation in each zone. MRI helps detect the cancerous tissue and its involvement with other nearby structures like the urethra, seminal vesicles, and the prostatic capsule, if any, depending on the changes in the intensity of signals.
Focal therapies such as IRE are at the cutting edge of medical innovation, as they reduce post-operative complications and damage to surrounding tissues.To treat cancer, needles are placed, together with an electric field, to cover the entire area of the tumour (volume) with a margin of 5mm and up to 10mm around the edge of the tumour visible on MRI. This ensures that all the cancer cells are destroyed, even if there is a small error in the MRI or biopsy results. Once the needles have been correctly placed, the trajectories and electrical distances are checked to avoid heating up and damaging neighbouring organs. The whole procedure takes around 45 minutes and can be carried out in a single visit to the hospital. Electrode positioning must be as precise as possible to obtain optimum results in complete safety.
Based on Cussenot’s studies on the geometric anatomy of the prostate applied to IRE, a tool (IRE Simulator) based on artificial intelligence has been developed by HDTECH to facilitate and optimise electrode placement for precise, effective and safe tissue ablation. In addition, the control of intraoperative thermocouples integrated into the needles, developed with HDTECH, avoids any risk of hyperthermia linked to variations in tissue conductivity or if inappropriate parameters have unfortunately been chosen manually by the surgeon (voltage, distance between electrodes, duration tissue pulsation, etc).
People with a PSA (prostate-specific antigen) less than 20, Gleason score (used to evaluate prostate cancer prognosis) less than 3–4, and unifocal lesion size less than 2cm are currently eligible for focal IRE application. Lesions less than 10mm in size can be treated easily with 4 IRE’s needles while those greater than 10mm (up to 15mm) need multiple configurations with electrodes.
IRE offers a number of advantages over conventional techniques such as cryo-ablation, radiotherapy, and hyperthermia. Unlike other partial ablation techniques, where it is difficult to operate close to functional anatomical structures due to the risk of necrosis (tissue death), the use of IRE reduces the risk of scarring of functional structures. This makes it possible to treat cancers close to the urethra, erectile nerves, or sphincter, which would otherwise lead to recurrence.
Thermal therapies (heat or cryotherapy), on the other hand, run the risk of damaging neighbouring tissues due to the non-specific nature of the treatment. This risk is also considerably reduced with IRE, which is more targeted and selective for the cancerous tissue. Unlike radiotherapy, which cannot be repeated in the same or neighbouring areas, IRE can be repeated.
Life after the IRE
Patients undergoing IRE must undergo an MRI scan 6 months after the procedure, along with the usual PSA test, and then every 12 months for at least 5 years. According to Cussenot, patients aged 50 and over have benefited from IRE with few or no side effects, and more than 80% of patients have had no recurrence of the disease during these biopsies.
Focal therapies such as IRE are at the cutting edge of medical innovation, as they reduce post-operative complications and damage to surrounding tissues, such as structures involved in erectile function and continence, and ensure the removal of cancerous tissue, thereby reducing the risk of recurrence. According to Cussenot, these advantages make IRE a safe and effective treatment modality for prostate cancer when detected at a low- or intermediate-risk stage, resulting in improved quality of life after the operation.
