COVID toe: A dermatological manifestation of COVID-19
Throughout the COVID-19 pandemic, different strains of the SARS-CoV-2 virus have resulted in a variety of clinical symptoms. As well as the more common respiratory symptoms, doctors also began to notice possible skin manifestations of the disease, which appeared similar to chilblain-type lesions. Dr Kazuhiro Komura of the Department of Dermatology, Kanazawa Red Cross Hospital, Japan, has explored the link between skin changes and COVID-19, and how this could be explained by underlying inflammatory and immune responses.
COVID-19 is a disease caused by infection with a coronavirus called SARS-CoV-2. The most common way that the virus is passed on is through small liquid particles or droplets that spread when an infected person coughs, sneezes, breathes, or speaks.
While most people infected with the virus will experience mild to moderate illness, some can become seriously ill. Vulnerable groups include older adults and those with underlying health conditions. Since the start of the pandemic in 2020, it is estimated that over 6 million people have died from infection with SARS-CoV-2.
Symptoms of COVID-19 vary widely, from general fatigue and cold-like symptoms, to severe respiratory distress. Less common symptoms may be related to skin symptoms, such as a rash. Dr Kazuhiro Komura at the Department of Dermatology, Kanazawa Red Cross Hospital, Japan, is interested in learning more about the relationship between skin lesions and COVID-19 disease.
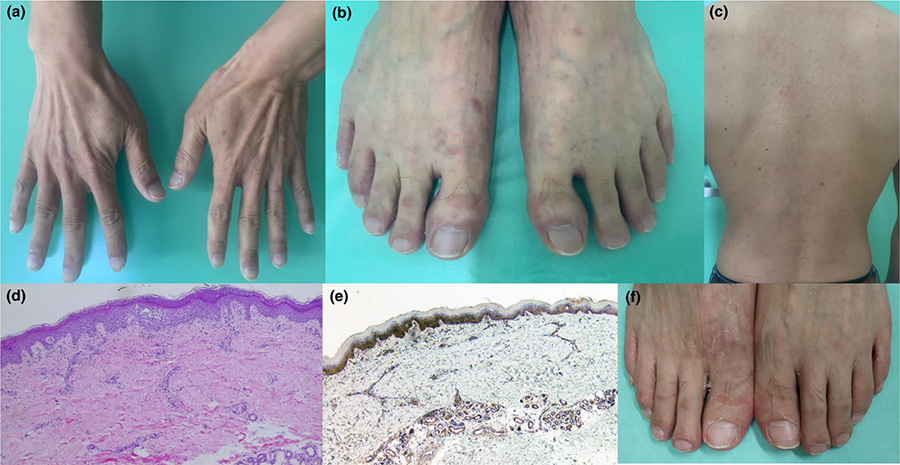
Skin lesions in COVID-19
Typical symptoms of COVID-19 tend to centre around respiratory issues; however, medical teams also began to notice acral erythema on the feet of some patients with COVID-19. Acral erythema is characterised by reddening, swelling, numbness, and sloughing of the skin and can be caused by chemotherapy or other medical conditions. Doctors found that these discoloured and swollen toes generally seemed to affect children and young adults who tested positive for SARS-CoV-2 infection at the initial stage of the pandemic. Most of these patients did not develop other, more classical symptoms of COVID-19 and generally appeared to have a milder form of the disease overall.
Komura describes a case study of one patient, a 49-year-old man who presented with skin lesions, fever, and headache. Blood results were generally all in the normal range, and an initial polymerase chain reaction (PCR) test for COVID-19 was negative. However, the patient did have antibodies against SARS-CoV-2 between days 25 and 45 after symptoms began.
The relationship between acral erythema and COVID-19 is complex, as only a minority of patients with COVID toe have positive PCR tests from the upper respiratory tract (nasal or throat swabs). One study shows this could be as low as 13 out of the 88 patients tested (15%). However, in another study, most patients showed positive COVID-19 results within the skin lesion (Colmenero et al, 2020). This suggests that SARS-CoV-2 may be distributed in other parts of the body, aside from the respiratory tract, and that patients with COVID toe may have a distinct pattern of viral infection compared to patients with more classic COVID-19 symptoms.
The role of signalling proteins
As well as linking skin changes to SARS-CoV-2 infection, researchers have also started asking how and why this phenomenon is occurring. Interferons are a group of signalling proteins that are made and released by cells in distress, such as those infected with bacteria, viruses, or cancer cells. These signals alert the immune system to a problem and help it identify the cause before launching the correct immune responses.
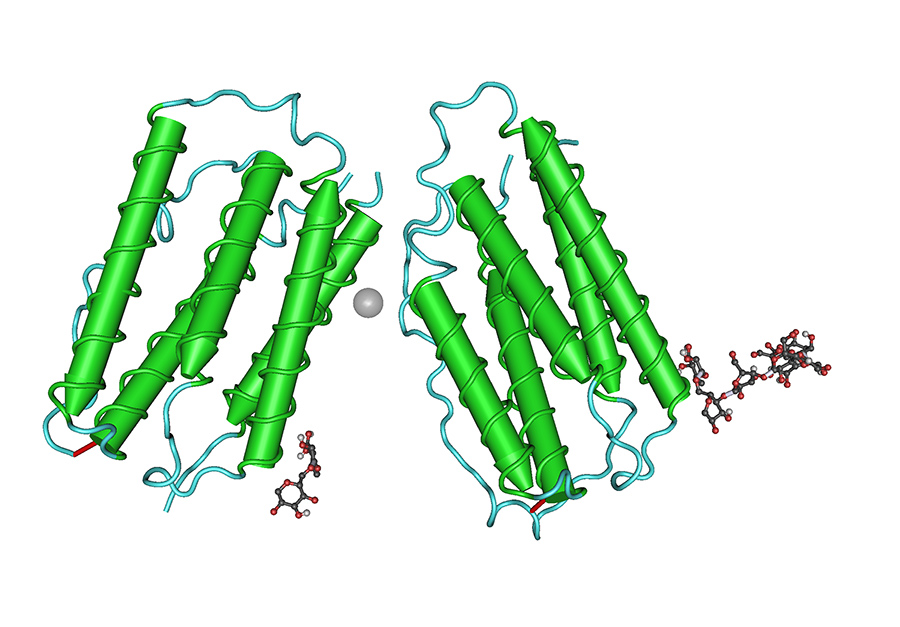
In particular, type 1 interferons (IFN-1) are associated with formulating effective immune responses to viral infections. It is already known that SARS-CoV-2 infection triggers a strong IFN-1 response to help protect the host. In addition, other diseases mediated by IFN-1 can be characterised by chilblains. Therefore, researchers are interested in learning more about the links between skin lesions occurring throughout the COVID-19 pandemic and lesions seen due to other conditions.
One example of this is a project done as part of the CORE (Covid Research) project, carried out by hospitals and institutes in Saint Louis, France. Here, researchers have explored the link between chilblain-like lesions (another way that acral erythema may be defined) in patients during the COVID-19 pandemic, type 1 interferons, and other cells of the immune system.
Patients with COVID toe may have a distinct pattern of viral infection compared to patients with more classic COVID-19 symptoms.
Their study included 50 patients with chilblain-like lesions (CLL) during the COVID-19 pandemic. Histological patterns were similar when COVID-19 related CLL were compared with seasonal chilblains; this means that when samples from the lesions were examined under a microscope, there was no difference in the structure of the tissue or the types of cell present between the two groups. There was also some overlap in the types of genes expressed in both patient groups, with genes encoding type 1 interferons being upregulated.
Overall, the study concluded a similar underlying pathophysiology between CLL and seasonal chilblains, with the strong IFN-1 response likely being caused by a viral trigger. They also suggested that using local or systemic inflammatory treatments, including IFN, could be one possible COVID-19 treatment.

Understanding the mechanisms behind COVID-19
A research group in Spain further explored whether CLLs were really indicative of COVID-19 and how this relationship could be better understood.
They evaluated all cases of acral lesions presenting to doctors’ offices during a three-week period and carried out a PCR test to see if they had COVID-19 at the time of these skin changes. Out of 58 patients, they found only one patient who tested positive (although 19 patients were not screened for COVID-19).
The same group also searched the literature to examine the findings of others around the world. In total, just 9 articles focused on acral lesions specifically. As this is such a new area of research, there was significant variation between the methods and results of the studies, making it difficult to compare them. For example, some studies looked at skin lesions in people infected with SARS-CoV-2 but did not compare this to findings in people without COVID-19, whereas others included data from skin lesions in people with and without COVID-19.
Komura concludes that skin lesions tend to be more commonly associated with milder forms of COVID-19. There is a possibility that they could be considered part of the diagnosis pathway for COVID-19, especially in areas where diagnostic tests are less accessible. However, due to the lack of research and understanding in this area, acral skin lesions should not be considered as a specific marker of SARS-CoV-2 infection in otherwise asymptomatic patients.
COVID-19 is still a very new disease and continually changes over time as new strains of SARS-CoV-2 emerge. Therefore, there is still much to be learnt about the disease and its symptoms, as well as the underlying mechanisms of infection. Understanding more about the virus will allow doctors and scientists to develop novel therapeutics or utilise existing treatment options, including IFN I, to offer the best care against COVID-19.
Personal Response
What are the next steps for this research?
First impression of COVID toes was very close to the looks of the familial chilblain, an inherited interferonopathy. Furthermore, IFN I is upregulated in seasonal pernio, systemic lupus, and SAVI, other hereditary syndrome presenting common peripheral skin appearance, within recent works. These have led us to consider that IFN I can cause skin symptoms during coronavirus infection. SARS-CoV-2 may have a distinct pathway of temporal augmentation of IFN I since usual viral infection causes IFN I overexpression without peripheral skin lesion. In this regard, ACE2, a specific receptor for SARS-CoV-2, may be involved in this relatively specific augmentation loop against SARS-CoV-2 infection. We hope to elucidate the relationship between ACE2, IFN I and SARS-CoV-2,and hope that specialists recognise/estimate the presence of COVID toes.