Early Action Review: Preventing local outbreaks from becoming pandemics
If we are to avoid the fallout of another global pandemic, we need to be better prepared. Dr Stella Chungong and Dr Landry Ndriko Mayigane of the Health Security Preparedness Department in the World Health Organization’s Health Emergencies Programme are encouraging countries to implement early action reviews (EARs) of disease outbreaks. EARs are based on a 7-1-7 metric to assess their vigilance, planning, and responsiveness, and could help countries be better prepared during outbreaks. Simple though the metric may seem, its demands are not – because the lives of millions may depend on it.
The COVID-19 pandemic, which rapidly escalated into a global crisis that impacted millions of lives and disrupted economies around the world, was a wake-up call for the management of infectious disease outbreaks. While the pandemic hammered home numerous hard lessons, two were fundamental: firstly, the benefits of global connectivity come with costs; and secondly, there is significant value in international collaboration with a common agenda.
Early action reviews (EARs) are a common and important public health tool that facilitate emergency response to communicable diseases and other public health events.The rapidity with which the coronavirus exploited weaknesses in global supply chains, international travel, and both regional and intra-urban transportation networks to spread surprised governments globally.
Nonetheless, scientists around the world swiftly collaborated to comprehend the virus and determine an effective strategy to combat it. While outbreaks and pandemics are inevitably bound to occur, future efforts must be focused on timely detection, notification, and rapid response to limit their impacts. Communication is critical, and a common language is vital.
Early Action Review
As part of the World Health Organization (WHO) Health Emergencies Programme (WHE), the Health Security Preparedness (HSP) department supports countries to continuously assess, monitor, and build national and sub-national capacities, through the development and implementation of national action plans for health security. However, recognising that each country has unique health priorities, Dr Stella Chungong and Dr Landry Ndriko Mayigane at HSP emphasise the importance of a unified global response to address international health security threats effectively.

Early action reviews (EARs) are a common and important public health tool that facilitate emergency response to communicable diseases and other public health events. In general, an EAR should be performed as soon as an outbreak is detected, as this allows for timely adjustments to response strategies. EARs can help mitigate the spread of the disease and strengthen readiness strategies by assessing the detection, surveillance, and early warning systems. Moreover, EARs are enhanced by early engagement with at-risk communities to bolster outbreak readiness. EARs prevent local outbreaks from becoming pandemics.

WHO published The Guidance for conducting an early action review (EAR) with the aim of offering a proactive assessment tool for evaluating preliminary strategies and actions for the early detection of outbreaks and identifying and addressing any gaps or shortcomings before outbreaks escalate. Timeliness and accountability are critical for this to happen, and a simple metric is needed to assess it.
The 7-1-7 metric
Among the hard lessons learned from COVID-19 were that surveillance and monitoring must be ongoing, early detection is crucial, collaboration must be global, reporting systems robust, public health infrastructure operational, risk communication clear, and response strategies adaptive. Based on these key factors, the new guidance provides granular, stepwise instructions for governments to implement EARs at different levels for various infectious disease contexts, with the aim of avoiding the outbreak from spreading and potentially becoming a global pandemic.
public health events.
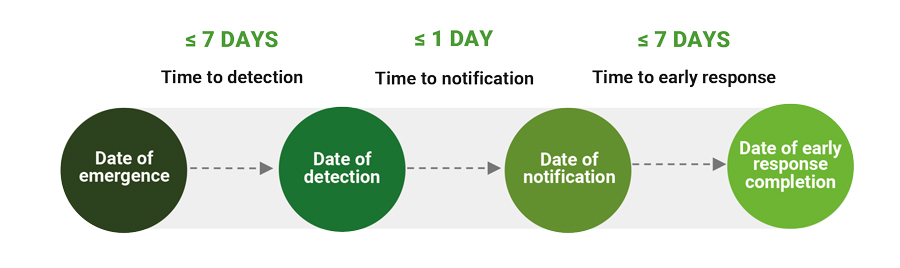
The guidelines detail three time-based metrics, named 7-1-7, which offer a simple, structured approach to outbreak management: (1) 7 Days to Detect, which measures how quickly the country can detect a suspected disease outbreak, with the aim being detection within 7 days, and (2) 1 Day to Notify, which measures the time taken to notify relevant public health authorities and stakeholders, with the aim being notification within 1 day. This goal is not new; it is consistent with the International Health Regulations (2005) that require countries to notify the relevant authorities within 24 hours of detecting a disease outbreak. Finally, (3) 7 Days to Respond measures how quickly the country can establish a response to the outbreak, the aim being the instigation of effective response actions within 7 days (Figure 1).
Drs Chungong and Mayigane acknowledge that simple though the7-1-7 metric may seem, achieving it may be challenging, especially for less-resourced countries.
The three-stage metric format has previously been applied for global initiatives against HIV and malaria. For example, the United Nations established a 90-90-90 goal for tackling HIV: 90% of people infected with HIV should know their status, 90% of those diagnosed receive sustained treatment, and 90% of those patients have undetectable viral load.
This approach ‘harmonised global action on solid, life-saving outcomes’, in part by generating enthusiasm and support; simple measures of progress are attractive to funders as they boast of clear, objective benchmarks (Freiden, et al, 2021).
Lessons from Africa
The 7-day target for detection is ambitious but doable and Africa is a case in point. It offers a good baseline for measuring detection, notification, and response because Africa hosts less-resourced countries with limited access to reliable laboratories. This is important because the detection component of the 7-1-7 metric is not a broad measure. It stipulates required capacities and response components during the 7-day target, including access to medical care, training healthcare workers to deal with a possible outbreak, and laboratory diagnostic capacity.
Africa is ground zero for many outbreaks. According to Drs Chungong and Mayigane, between 2017 and 2021, the WHO African region reported 589 acute public health events – the highest among all WHO regions. Such a high number has made the continent something of an old hand at outbreak detection. A WHO review of 296 substantiated human and animal disease outbreaks in the African region from 2017 to 2019 showed a median of 8 days for time to detection and 3 days for time to notification.
Becoming more adaptive
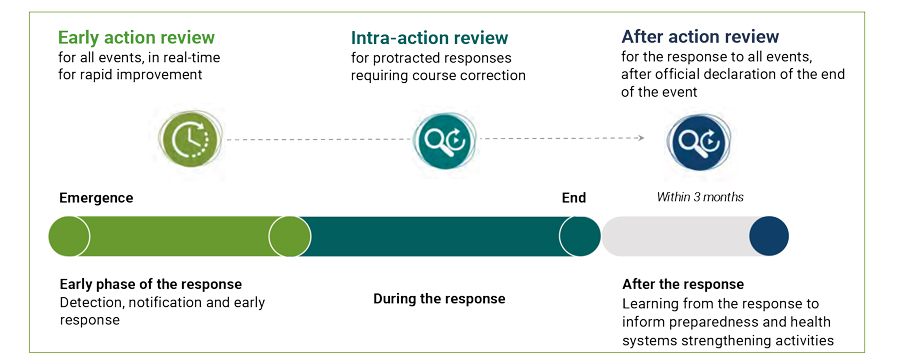
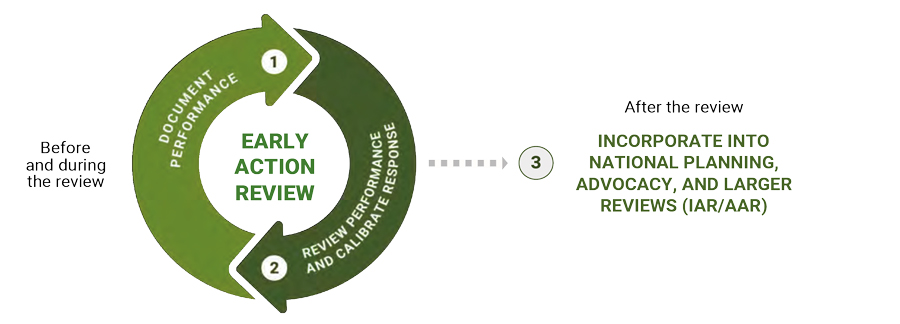
EARs are supplemented by subsequent intra-action reviews (IARs), which employ real-time assessment methods and are conducted during the response, and after action reviews (AARs), which provide retrospective analysis (Figure 2). Together, the information from these initiatives provides critical insight for future emergencies and can be incorporated into national and regional policy strategies (eg, Integrated Disease Surveillance and Response in Africa, the Asia Pacific Strategy for Emerging Diseases) and improve future responses (Figure 3).

EARs are also a valuable resource to support other WHO initiatives. For example, they provide a robust dataset to support the global health architecture for Health Emergency Preparedness, Response and Resilience.
EARs also align with the One Health approach, which was established to improve the integration of work on human, animal, and environmental health. In particular, many health issues, including outbreaks of certain infectious diseases, are linked with environmental factors and animal health – for example, zoonotic diseases, which can spread between animals and humans. As such, effectively addressing them requires informed input from those working in human medicine, veterinary medicine, environmental science, and public health. With better communication and sharing of knowledge, more effective and timely surveillance systems, data sharing mechanisms, and coordinated responses can be established.
Proactive, not reactive
Drs Chungong and Mayigane acknowledge that simple though the 7-1-7 metric may seem, achieving it may be challenging, especially for less-resourced countries. Identifying and tracking a potential outbreak in remote areas of countries with limited access to reliable laboratories for differential diagnosis can hamper detection. Fear of triggering a false alarm can delay notification, and the response components are demanding. However, progress of any kind can build capacity and resilience.

By providing countries with guidance that incorporates a straightforward and simple-to-communicate but thorough metric for timeliness and accountability in detection, notification, and response, WHO is helping countries become more adaptive, thereby preventing local outbreaks to convert into pandemics. As the researchers conclude – ‘In a world that is increasingly susceptible to large-scale health emergencies, being proactive rather than reactive saves lives, resources, and preserves the integrity of our health systems’.
Personal Response
What could be the most common challenge for countries – especially those less resourced – to achieve the 7-1-7 target in an early action review, and what could be done to address this?The lack of infrastructure and resources to collect, analyse, and act upon the data efficiently. This 7-1-7 metric, which likely involves timely diagnosis, reporting, and response to health issues, requires robust health information systems, trained personnel, and adequate funding. To address these challenges, international cooperation and support are crucial. Partnerships with global health organisations can provide the necessary technical support, training, and financial resources to strengthen local health systems. Additionally, leveraging mobile technology and community health workers can be cost-effective strategies to improve surveillance and response capabilities in resource-limited settings.