Case for the improvement of suboptimal care of gout patients in Hawai’i
Gout is a joint condition which develops as a result of excessive levels of uric acid in the blood. It is a form of inflammatory arthritis (disease of joints characterised by pain, swelling, stiffness and inflammation) which occurs when uric acid forms needle-like crystals that become deposited in a joint. This gives rise to sudden, severe pains in the affected joint. Parts of the body which are commonly affected include the big toe, knees, elbows, where the skin over the joint becomes red, hot and swollen in episodes referred to as gout flares.
According to Lim et al. (2016), gout is one of the most common inflammatory joint conditions, but other forms of inflammatory joint conditions like rheumatoid arthritis (RA) are also prevalent. RA is an autoimmune disease (a medical condition which occurs when the body immune system attacks normal body tissues). It is unclear what triggers this unusual body reaction in patients with RA but the immune system mistakenly attacks the lining of joints, causing them to swell and become painful and stiff. In RA there are chronic joint pains, but frequently joint flares occur as in gout, during which symptoms may become worse.

The burden of gout in Hawai’i
With increasing levels of adiposity, hypertension and high rates of diuretics utilisation worldwide, the prevalence of gout has increased significantly. In a study by Zhu et al. (2011), 3.9% of US adults were diagnosed with gout between 2007 and 2008. Emergency department visits due to gout flares cost approximately 3.4 times more than regular gout outpatient visits. In the same vein, the number of hospitalisations due to gout in the United States between 1993 and 2011 increased while rheumatoid arthritis hospitalisations decreased, according to the study by Lim et al. (2016). The average cost for hospitalisation for gout is approximately 6000 dollars. Although previous studies in the United States have highlighted the rising incidence of gout, increasing cost of emergency department visits and hospital admissions, there has been no comprehensive research on the healthcare utilisation of gout patients in the Pacific region and Hawai’i. The racial composition of Hawai’i is different from the rest of the United States. Hawai’i has higher proportion of Pacific Islanders, Asians and other multi-ethnic groups, many of which are thought to have higher uric acid levels, making them more susceptible to gout.
When patient compliance with medication is combined with lifestyle changes, lower levels of uric acid can be achieved with the prospect of fewer gout flares.
Gout is eminently treatable, and emergency department visits and hospitalisations can be reduced if care for gout patients in Hawai’i is improved. It therefore becomes imperative that the disease burden of gout in this region be assessed so that health policies geared towards the improvement of care for gout patients be put in place.
Highlights of the study
Dr Lim and his colleagues did just that in their study in 2019. The study highlights the critical deficiencies in the care of gout patients compared to RA patients in Hawai’i. Between 2011 and 2017, gout patients visited the emergency department more often than rheumatoid arthritis patients, likely due to more episodes of gout flares arising from suboptimal care for gout patients. Near absence of data specific to the region presented significant challenges to the comparison of healthcare utilisation patterns for both groups. A retrospective chart review of both gout and RA patients was therefore undertaken. Dr Lim and his co-authors had access to identifying information by reviewing patients’ medical records at Hawai’i Pacific Health, which is one of the largest healthcare providers in Hawai’i.

Included in the study were patients 18 years and above who had encounters (attended an outpatient setting, emergency department or were hospitalised) with any of the various facilities of Hawai’i Pacific Health healthcare system with a diagnosis of gout on discharge. They also must have had a follow-up data of at least one year at the time of the study. The RA group of patients was selected for the study to enable comparative analysis of gout healthcare utilisation patterns be made with that of a similar inflammatory arthritides.
The results revealed that between 2011- 2017 there were a total of 9552 encounters (comprising of outpatient visits, inpatient admissions, and emergency department visits) with a primary discharge diagnosis of gout. In comparison, there were a total of 7272 encounters with a primary discharge diagnosis of RA within the same period.
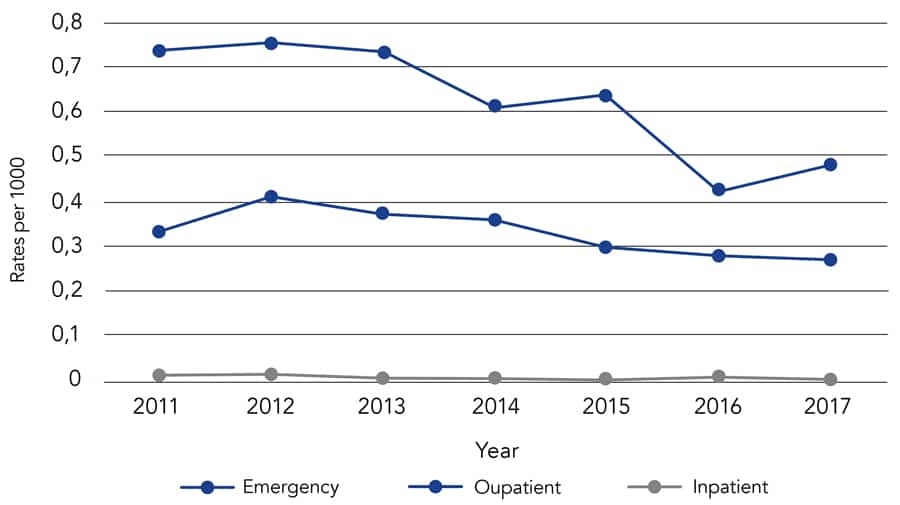
Although the annual rates for emergency department visits and outpatient visits were trending lower and inpatient admissions remained stable over the period for gout patients, the group recorded a high rate of emergency department visits.
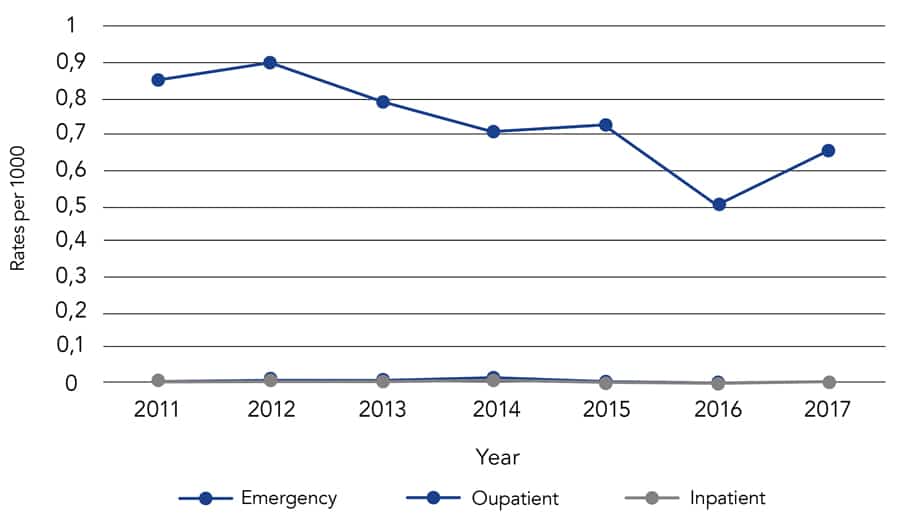
In contrast, RA patients had very low and stable admission rates during the study period, and most of the healthcare utilisation centred mainly on the outpatient setting with practically little or no emergency department visits.
The study also compared the costs of outpatient visits, inpatient admissions and emergency department visits of gout patients with those of the RA group. The study revealed that in 2017 for example, the mean cost for every emergency department visit by a gout patient was approximately 3.4 times the cost of an outpatient visit. In the RA group, an emergency department visit cost approximately 3.5 times the cost of an outpatient visit during the same year.
Although emergency department utilisation rates for gout patients declined between 2011 and 2017, the emergency department visits represented a significant portion of healthcare utilisation for gout patients while RA patients were managed mainly in the outpatient setting. Since emergency department visits are associated with higher costs than outpatient visits, efforts must be made to reduce the healthcare costs of gout patients by facilitating the outpatient evaluation of gout patients and reducing emergency department utilisation.
With increasing levels of adiposity, hypertension and high rates of diuretics utilisation worldwide, the prevalence of gout has increased significantly.
Recommendations for improved care for gout
Many emergency department visits by gout patients can be prevented if gaps in the management of chronic gout can be filled. Better access to care will go a long way in reducing emergency department visits, especially during a gout flare. Establishment of urgent care clinics and extension of primary care operating hours will reduce unnecessary emergency department visits and hospitalisations.
Gout patients are often treated by primary care physicians. Training physicians in primary care settings to improve their knowledge of gout flare management and development of systems to manage patients with gout efficiently will improve level of care. In this regard, it is essential that healthcare providers manage gout strictly according to national guidelines. Serum uric acid levels should be actively monitored by physicians to prevent gout flares.

Gout patients have their own role to play in cutting down the number of emergency department visits and reducing the cost to the healthcare system. Here, patient education is essential to improve medication compliance. Healthcare providers must engage with their patients and have discussions with them on lifestyle changes. Buttressing this fact, Dr Lara Pullen in an article in the online publication, The Rheumatologist, pointed out that these advice ‘can include suggestions on obesity, alcohol use, fructose consumption and the consumption of purine-rich fatty foods’. This will help improve the patient’s lifestyle and cut down the burden of gout on the healthcare system. When patient compliance with medication is combined with lifestyle changes, lower levels of uric acid can be achieved with the prospect of fewer gout flares.
Conclusion
Gout patients in Hawai’i have a high number of emergency department visits which is associated with significant cost to the healthcare system. As gout is a treatable disease, efforts should be made to implement the recommendations in this study to improve the suboptimal care of gout patients in Hawai’i with a view to reducing the burden on the healthcare system.

Personal Response
What would be the modalities for ensuring that the findings and recommendations emanating from this study are implemented by health authorities in Hawai’i?