Significance of patient positioning guidelines in endoscopic procedures
Patients are placed on an operating table for surgery or, in the event of endoscopic treatment, on a trolley. Surgery may need patient placement that is not at all comfortable, posing challenges for the patient. There are well-established rules for patient positioning during surgical operations, but no such criteria are available for endoscopic treatments. A study conducted by Dr Vera Meeusen and her team from Princess Alexandra Hospital, University of Queensland, demonstrates it is possible to apply most of the patient-positioning guidelines for surgical procedures to gastrointestinal endoscopic procedures in endoscopy units.
Surgery may need patient placement that is not at all comfortable, posing challenges for the patient. Patients may experience discomfort as a result of overstretched muscles, lying on something hard or against something sharp. They can also experience overstretching or compressing nerves and squeezing skin tissue, which can result in temporary or permanent injuries/damage. Patient positioning (PP) involves placing the patient on the operating table (or trolley) in such a way that the doctor can complete the procedure while the patient remains comfortable. There are well-established rules for PP during surgical operations, and nurses and surgeons are well-versed in how to follow them.
Unfortunately, endoscopic treatments do not have these criteria. Endoscopy is a procedure where organs inside the body are looked at using an instrument called an endoscope. Gastrointestinal endoscopists and endoscopy nurses do not receive training in patient positioning safety. Dr Vera Meeusen and her team from Princess Alexandra Hospital, University of Queensland, have tested whether the existing guidelines of patient positioning can be applied to the endoscopic procedures. Correct posture seeks to ensure safety and efficiency while also considering the patient’s subsequent wellbeing, such as limiting the risk of nerve and tissue damage.

The need for patient positioning in endoscopic procedures
Traditionally, gastroenterologists in endoscopy units perform diagnostic endoscopic operations under procedural sedation or without any patient sedation. The majority of the caseload consists of diagnostic gastrointestinal endoscopic operations that last 30–60 minutes on average. This could explain why, in contrast to surgical procedures performed in the operating room, patient placement has received little attention in endoscopy. Advanced endoscopic interventions (eg, peroral endoscopic myotomy and endoscopic sleeve gastroplasty) have become established in expert centres over the last few decades, with procedure times exceeding 60 minutes and in some cases lasting several hours, and frequently requiring general anaesthesia. Peroral endoscopic myotomy (POEM) is a minimally invasive endoscopic procedure intended for long-term recovery from symptoms of oesophagal achalasia (benign motility disorder). Endoscopic sleeve gastroplasty is a newer type of minimally invasive weight-loss procedure.
Endoscopy units are facing new challenges as the number of complex and lengthy advanced procedures performed on patients with comorbidities and obesity rises.
Obese patients are more likely to have medical conditions such as atherosclerosis (hardening and narrowing of the arteries), arthritis, sleep apnea syndrome (a potentially serious sleep disorder in which breathing repeatedly stops and starts), alveolar hypoventilation (a rare condition in which a person does not take enough breaths per minute), urinary stress incontinence (unintentional loss of urine), and gastroesophageal reflux disease (a condition in which acid-containing contents in your stomach persistently leak back up into your oesophagus, the tube from your throat to your stomach). These conditions can increase the risk of patient injuries, reduce tissue perfusion (blood flow), and jeopardise safe positioning. Specialised equipment is required for these patients (eg, sideboards attached to the operating table, extra-wide and extra-long safety belts, a ramping posture, and an adjustable bed/stretcher capable of weight support).


Patient positioning in the lateral position can be challenging due to a lack of competency and suitable positioning devices.
Endoscopy units are facing new challenges
The proper posture of surgical patients in an operating theatre has garnered a lot of attention for a long time. Surgical practice guidelines are widely available, and anaesthesia and perioperative nursing professionals receive instruction in patient posture as part of their education. The goal of the recommendations is to avoid exposing body surfaces to too high and prolonged pressure, which is the underlying concept that leads to pressure injuries. This can be performed by using pressure-relieving beds or cushions, as well as proper patient positioning. Evidence reveals that patient positioning in lateral and prone positions can be challenging due to a lack of competency among nurses and porters, as well as a lack of suitable positioning devices. Despite the widespread availability of patient positioning guidelines for surgical procedures, neither the American Society of Gastroenterology Nurses and Associates, the Gastroenterological Nurses College of Australia, nor the European Society of Gastroenterology Nurses and Associates mentions patient positioning during gastrointestinal endoscopic procedures in their standards, guidelines, or publications.


Left-lateral patient positioning.
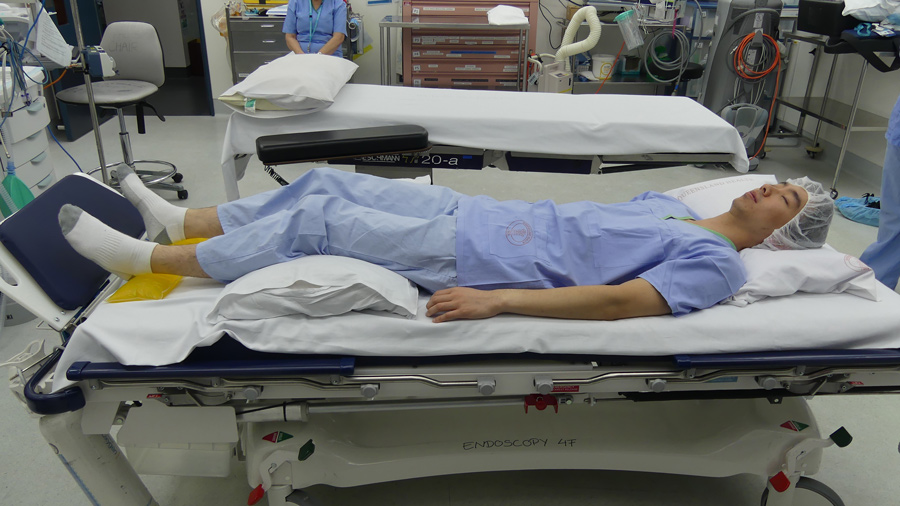
During endoscopic operations, the supine, left lateral, and prone positions are currently the preferred methods of patient positioning. Supine position is used in the majority of surgical procedures. A range of surgical procedures, including thoracic, hip, and shoulder surgery, are performed in the lateral position. Several forms of surgery, including brain and spinal surgery, are performed in the prone position.
However, depending on the pressure and nerve-injury avoidance measures used, these positions can produce nerve injury, skin damage, or compression of tissue or vascular systems, resulting in localised ischemia – a condition where parts of the body aren’t getting enough blood (and thus oxygen). The increased occurrence of these injuries in patients with obesity and related comorbidities can increase the risk of these injuries even more. The prone position during endoscopic treatments has several advantages for the proceduralist and anaesthetic team, including reduced risk of aspiration, easier access to the oropharynx and oesophagus, and allowing the endoscopist to face the patient directly. Endoscopy units are facing new challenges as the number of complex and lengthy advanced procedures performed on patients with comorbidities and obesity rises. Surgical positioning practice recommendations are therefore all the more important.

The goal of Dr Vera Meeusen and her team’s study was to see if patient placement standards for surgical operations in operating rooms might be used for gastrointestinal endoscopic procedures without compromising safety or length of time. They investigated the feasibility of three patient groups: those with a low body mass index (BMI 18.5 kg/m2), those with a normal BMI (BMI 18.5–24.9 kg/m2), and those with a high BMI (BMI >35 kg/m2). Three volunteers were found among hospital workers, one for each BMI group, with BMIs of 18 kg/m2 (male), 23.5 kg/m2 (female), and 43 kg/m2 (female).


Patient in the prone position (left) and swimmer’s position (right), a modified semi-prone position.
The research project was split into two parts. First, the volunteers were placed on the operation table in the supine, lateral, and prone positions, as recommended by best-practice patient-placement recommendations. Gel mats, gel rolls, cushions, and arm boards were used for safe positioning. The participants were asked to rate their level of comfort after they were positioned, and photographs of the actual positioning were taken. Second, the volunteers were placed on the endoscopic patient stretcher in the supine, lateral, and prone positions using the same recommendations.
Establishing positioning standards for endoscopic procedures in the supine, prone, and lateral positions is critical.
During the second phase, an endoscopist was asked to check for oral access. The volunteers’ positions were altered according to the endoscopist’s instructions, while still attempting to follow the patient positioning criteria for surgical operations in operating rooms. The level of comfort was measured once more, and photographs were taken. When comparing patient postures on the operating table and the endoscopic stretcher, however, the level of comfort was scored differentially between the BMI groups.
This study demonstrates that it is possible to replicate patient positioning guidelines for surgical procedures in gastrointestinal endoscopic procedures in endoscopy units, except for arm positioning in lateral and prone positions, and head positioning in the prone position. Both supine and lateral posture were found to be equally comfortable by all participants. When compared to the other positions on the endoscopic stretcher, the obese volunteer felt much less comfortable in the prone position. The prone position was the most difficult for endoscopists to work with. It was impossible to put the head in a neutral forward posture because it would restrict the endoscopist’s access to the mouth. The head was put on the edge of the pillow and turned laterally to improve mouth access, while the height of the head was kept in line with the cervical spine. Volunteers felt most ease in the prone position with their head aligned with the cervical spine and slightly turned to the right, left arm next to the body, and the elbow of the right arm flexed with the hand at the height of the shoulder line. The so-called swimmer’s position, a modified prone (semi-prone) position, was also investigated. Placing cushions under the right side of the volunteers’ thorax and abdomen, creating a prone 30° lateral-tilt position, was the most pleasant choice.
Looking ahead
Establishing positioning standards for endoscopic procedures in the supine, prone, and lateral positions is critical. The new guidelines for patient placement during gastrointestinal endoscopic procedures should be included in national endoscopy practice standards and endoscopy nurse education. The present rules for patient positioning in operating rooms during surgical operations could be used as a guide. Real-world research with real-world patients during real-world endoscopic operations is required. More study is needed to establish a method to estimate the best size of gel roll for each patient’s rib cage in the lateral position.

Personal Response
What suggestions do you have for researchers investigating and trying to identify the most suitable patient position for gastrointestinal endoscopic procedure?
• Most urgently is the optimisation of the prone position. We have recently finalised a study regarding the prone and semi-prone positioning during ERCP procedures.
• More research is needed on whether there is a need for special gel mats/pillows to improve oral access and positioning of the arms.
• Further research is also needed to establish safe work instructions in how to apply patient positioning without the requirement of physical heavy manual handling by healthcare practitioners. Aids used in theatre to transfer patients from bed/trolley to operating table are not suitable for endoscopy. Currently, patients self-position or are lifted by nurses and porters (especially obese patients).