Antimicrobial stewardship programmes: Remote consultations can help reduce antibiotic resistance
The increased use of antibiotic therapy to treat infectious diseases is driving up antimicrobial resistance as well as economic and healthcare costs. Antimicrobial stewardship programmes are crucial to monitor and evaluate medication use. Valéria Cassettari, Newton Novato, and Maria Helena Flesch Onuchic at NotreDame Intermédica Advanced Outpatient Clinic in São Paulo, Brazil, explored the impact of remote consultations with an infectious disease physician on antimicrobial regimens in outpatients. Their work showed that many prescriptions need amending, highlighting the importance of rigorous prescribing guidelines and regular review of antimicrobials to allow the drugs to be used as effectively and safely as possible.
Infectious diseases are caused by microorganisms such as viruses and bacteria. They encompass illnesses that are not transmittable to someone else, such as urinary or orthopaedic infections, or ones that are contagious, such as measles. In 2019, 13.7 million people worldwide died from infectious diseases, with respiratory and bloodstream infections being the most dangerous.

Antimicrobials are a group of medicines used to treat these infections – they include antibiotics as well as antiviral, antifungal, and antiparasitic drugs. However, microorganisms can adapt and evolve over time and often develop ways to avoid being killed by these drugs. This antimicrobial resistance (AMR) makes infections much harder to treat and drives the use of multiple medications to manage the disease.
Combating antimicrobial resistance
There is a higher risk of others getting ill and greater levels of death and severe illness if medications are less effective at clearing dangerous organisms from the body. The World Health Organization estimates that there are around 4.95 million deaths globally each year associated with AMR, most of which affect low- and middle-income countries. In 2019, AMR was described as one of the top ten global threats to public health, highlighting just how important it is to manage this development.
Several strategies can be used to combat AMR. Firstly, vaccines that prevent people from getting infections in the first place reduce the need for antimicrobial drugs further down the line. Secondly, developing novel drugs means that microorganisms don’t have time to develop resistance against them. Lastly, using existing medications carefully to avoid driving AMR can also help.
Using medications carefully and in accordance with prescription guidelines has health benefits by itself. Indeed, overuse of antimicrobial medications can lead to health complications such as allergy, diarrhoea, and kidney failure. There is also a financial burden; poorly chosen antimicrobials may be ineffective at clearing an infection, meaning that multiple courses of different medications are required to treat the illness.
Given the extent of the problem, methods to guide and monitor the use of antimicrobials are vital. In light of this, antimicrobial stewardship approaches have been developed.
Antimicrobial stewardship
Valéria Cassettari, Newton Novato, and Maria Helena Flesch Onuchic at the NotreDame Intermédica Advanced Outpatient Clinic in São Paulo, Brazil, point out that antimicrobial stewardship actions have been implemented in hospitals for nearly 30 years. In contrast, there is less control over medications used at home once a patient has been discharged from hospital.
For example, intravenous antibiotics can be used at home and administer drugs straight into the bloodstream. This is also called outpatient parenteral antimicrobial therapy (OPAT) and is an approach which has increasingly been used in recent years, as healthcare services aim to support people at home and reduce the length of their stay in hospital. With the rise in antibiotic resistance and a decrease in antibiotic options, there has also been an increase in the use of OPAT to try to combat these infections.
A few years ago, the Brazilian health maintenance organisation, NotreDame Intermédica, showed a steady increase in the use of intravenous antibiotics at home. This led to the launch of the antimicrobial stewardship programme in 2019, developed to assess the appropriateness and usage of OPAT over a period of 11 months.
In 2019, antimicrobial resistance was described as one of the top ten global threats to public health.The programme was led by a doctor specialising in infectious diseases, who carried out remote consultations through email, telephone, and a messaging platform. A review of antimicrobial medication use could be requested directly by doctors prescribing the drugs as well as nurses who scheduled home care. The specialist doctor used clinical information about a patient, alongside measurements of renal (kidney) function, weight, culture test results, and previous antimicrobial use to advise on a clinical plan. The doctor reviewed each case and passed on their recommendations to the outpatient clinic or discharging hospital responsible for the patient’s care.
The specialist doctor only suggested changes if any concerns were identified, such as an inappropriate antibiotic for the bacteria identified through testing, availability of an equally effective oral antibiotic, high risk of toxicity, incorrect dosage instructions, or the availability of a cheaper medication with the same effectiveness. These changes were not mandatory but could be implemented by the primary care provider if they wished and were based on two academic clinical manuals, both of which are routinely used in clinical practice in São Paulo.
Identifying the best medication for the job
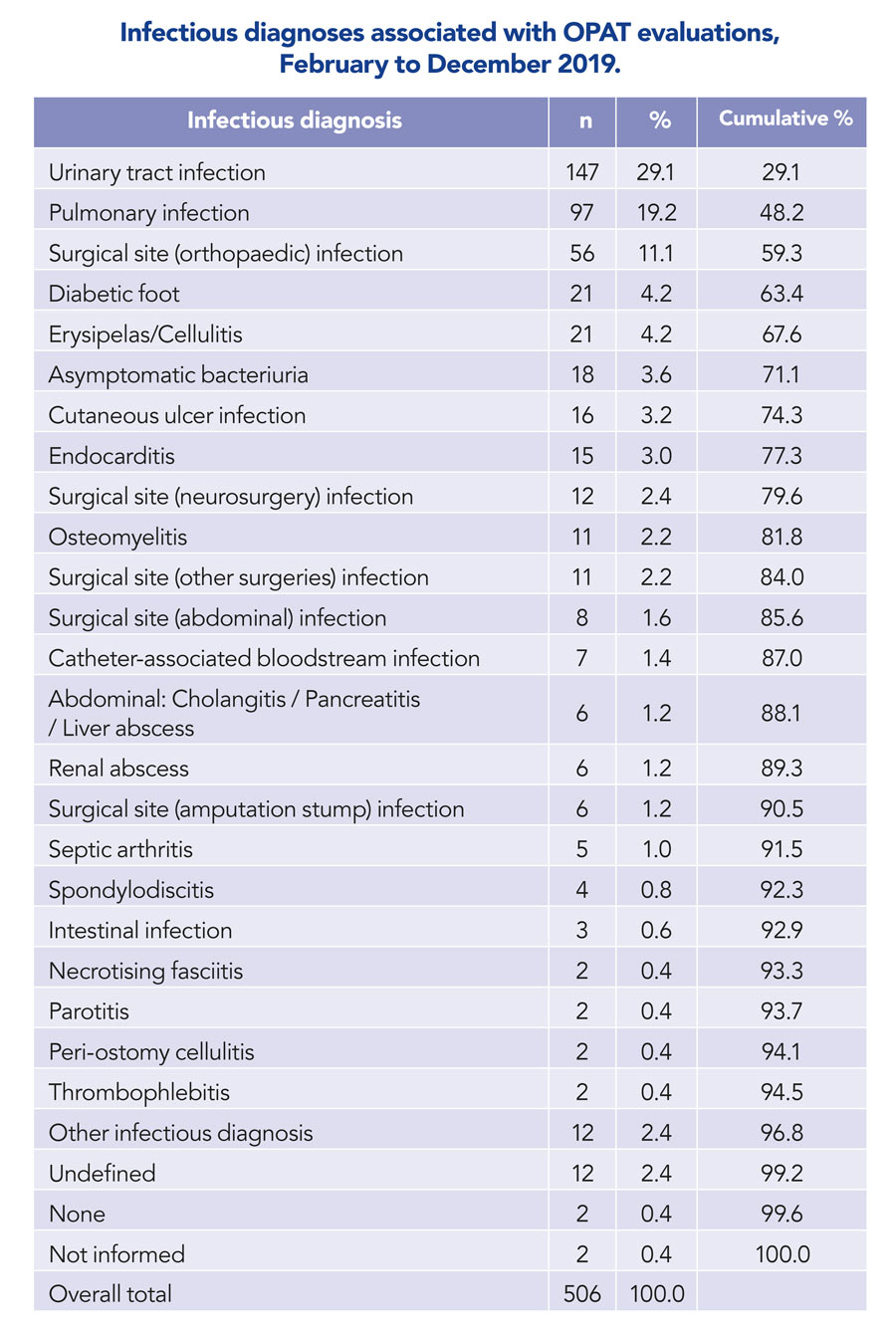
Cassettari, Novato, and Onichic report that a total of 506 requests for antimicrobials were evaluated. The most frequent illnesses for which antibiotics were prescribed included urinary tract infections, pneumonia, and hospital-acquired infections following orthopaedic surgery. Around half of the patients were over 65 and the number of assessments increased for older patients. Patients between 45–64 years old were mainly male, whereas patients over 85 years old were more likely to be female.
There were some cases where there was insufficient information to carry out a review and some requests for initiation of antimicrobial therapy, rather than a review of an existing plan.
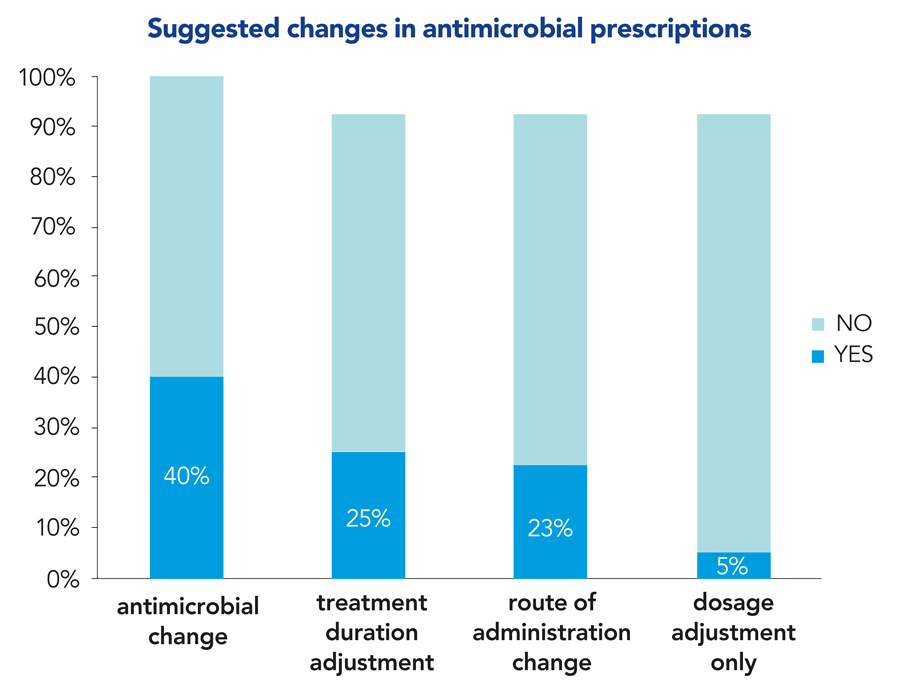
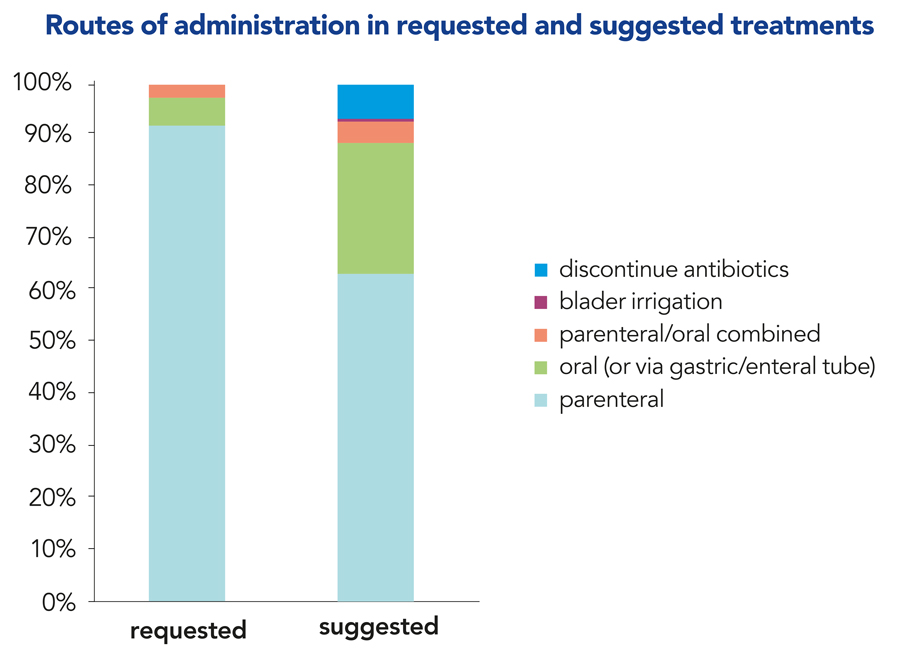
Of the 416 assessments carried out, antimicrobial prescriptions were approved with no changes in 42% of cases. After being reviewed by the specialist physician, modifications were requested in the remaining 58% of cases, with the most frequent changes being a different antimicrobial medication (40%). Other advised changes included treatment duration (25%), route of administration (23%), and dose adjustment (5%). For example, the average duration of treatment in the suggested plan was 13.3 days, compared to 16.9 days in the original care plan.
Although many patients were advised OPAT, the antimicrobial regimens recommended by the specialist doctor tended to trend towards oral therapies. There was also a significant proportion of revisions to the diagnosis of infection and duration of treatment, and the doctor suggested discontinuing antimicrobial treatment in 7% of cases.
Many patients had laboratory investigations to explore what type of microorganism was responsible for the illness, as the characteristics of the growing culture (a plate or tube with the right conditions for organisms to grow) can be used to identify the specific microbe. Where an infectious agent was identified, the specialist doctor considered 23% of prescriptions to be inadequate and requiring further review.
Detailed notes were kept for each treatment evaluation in the study, so that Cassettari, Novato, and Onuchic were able to review what happened following any recommended changes to antimicrobial regimens. There was a very low rate of treatment failure, with only 2 cases (0.4%) failing to show improvement following review. Both these treatments were then amended which led to favourable outcomes. Although no serious adverse outcomes were identified for any patients involved in the programme, the research team explains that these two failures show the need for rigorous intervention criteria as well as possible limitations of using remote evaluations rather than face-to-face appointments.
Changes in pharmacy prescriptions
In addition, the study reviewed data from pharmacies to see how these clinical recommendations translated into medication usage. The researchers were able to show a downward trend in the number of antimicrobial prescriptions after the introduction of the stewardship programme. In previous years, the monthly OPAT dispensing rate had been increasing.
Where an infectious agent was identified, the specialist doctor considered 23% of prescriptions to be inadequate and requiring further review.The work done by the group at NotreDame Intermédica Advanced Outpatient Clinic highlights the need for antimicrobial stewardship programmes to review and refine medication regimens of patients at home or in a care facility. Their study concludes that remote consultations by a doctor specialising in infectious diseases are safe and effective in the home care setting and does not require additional technological resources to undertake the reviews.
Using the most appropriate therapeutic approach will improve effectiveness, reduce health and financial costs, and slow the development of antimicrobial resistance. Management strategies must take into account the needs and resources of healthcare services, but could have huge benefits for patients and prescribers alike.
Personal Response
How could the findings of your work be integrated into healthcare systems?Remote consultation by an infectious disease physician can improve the prescriptions of intravenous antibiotics to be administered in home care. To implement this practice efficiently, healthcare managers must encourage collaborative communication between physicians prescribing antibiotics and an experienced infectious disease specialist. All clinical and laboratory information for each case, as well as the opinions of the professionals involved, need to be shared, which is why an environment of trust and efficient and continuous communication channels are important. It is also necessary to define protocols on which treatment decisions are based. Recording and periodic reevaluation of interventions are necessary to ensure their safety.