Bidirectional relationship between chronic pain and insomnia
Dr Aubrey Husak, internal medicine resident at the Ohio State University, and Dr Matthew Bair, Core Investigator at VA HSR&D Center for Health Information and Communication and Associate Professor at Indiana University School of Medicine, carried out a review on the bidirectional relationship between chronic pain and insomnia. They found common comorbidities, including depression, anxiety, suicidal ideation, and catastrophising. Patients with both chronic pain and insomnia were also more likely to have worse pain symptoms than individuals who do not experience insomnia. It was found that pregabalin improved pain and insomnia symptoms while cognitive behaviour therapy for insomnia showed long-term sleep improvements for patients with chronic pain. Concurrent treatments should be explored in future investigations to tackle both chronic pain and insomnia.
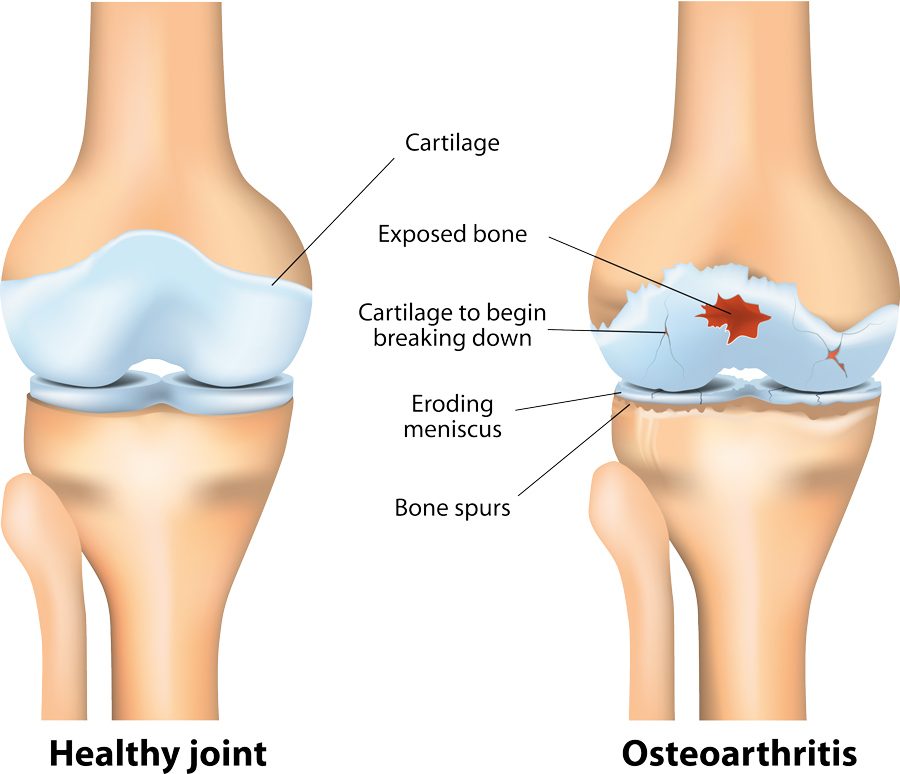
Both chronic pain and insomnia represent major challenges to global public health and healthcare systems. Chronic or persistent pain is defined as pain that lasts for more than 12 weeks despite medical intervention. It affects people living with a range of diseases, including osteoarthritis (pain and stiffness of the joints) and low back pain. The Diagnostic and Statistical Manual of Mental Disorders (DSM) defines insomnia as the difficulty with falling and/or staying asleep, which results in a poor quality of sleep. Frequent transient wakefulness and prolonged periods of wakefulness can deeply impair an individual’s day-to-day schedule. For diagnosis, individuals have to experience sleep disturbances for at least three days per week for at least three months. The prevalence of chronic pain has been estimated to exist in 17-25% of the general population, whereas approximately 10-15% of individuals live with insomnia.
24-32% of patients with chronic pain also report experiencing insomnia, as defined by the DSM. This is double the proportion of individuals in the general population. In addition, when insomnia is more broadly defined, the incidence of individuals living with both chronic pain and insomnia increases to a range of 40-80%. This signifies that patients with chronic pain are more likely to exhibit symptoms of insomnia.

People experiencing chronic pain and insomnia are more likely to have higher incidences of depression, anxiety, and fatigue. The strong relationship between chronic pain and insomnia, along with similar comorbidities, require further investigation to elucidate better treatment for this patient population. Previously, it was assumed that insomnia is directly caused by chronic pain and alleviation of chronic pain will also treat insomnia-related symptoms. However, researchers recently theorised a bidirectional relationship, which states that chronic pain and insomnia exist together and can exacerbate each other.
Resolution of sleep disturbances was more likely to be followed by reports of lower pain intensities.
Literature review
Dr Aubrey Husak, internal medicine resident at the Ohio State University, and Dr Matthew Bair, Core Investigator at VA HSR&D Center for Health Information and Communication and Associate Professor at Indiana University School of Medicine, set out to write a review that answers three questions to fill in the gaps on the relationship between chronic pain and insomnia:
- How does concurrent chronic pain and insomnia affect the severity and pain duration in patients with chronic pain?
- What are the common comorbidities and pain-related symptoms in patients with both chronic pain and insomnia?
- What are the potential treatment options for both chronic pain and insomnia?

Two databases of research papers, OVID Medline and PubMed, were searched from 1946 to June 2017 for the topics ‘chronic pain’ and ‘sleep disorders’, with an emphasis on treatment. This search yielded 313 articles, but only 33 were included after eligibility checks. Participants that did not meet the DSM criteria for insomnia were included in the review, as these individuals can still experience symptoms that are life-debilitating. However, other related medical conditions such as sleep apnea and restless leg syndrome were not included in the review. The term chronic pain was broadly searched for, which yielded conditions like fibromyalgia (a long-term condition that causes widespread pain all over the body; thought to be caused by the way the nervous system processes pain signals) and osteoarthritis. Only randomised controlled trials that assess the effectiveness of treatments were included.
Dr Husak and Dr Bair’s review found that there was a bidirectional relationship between insomnia and chronic pain. Better sleep quality was correlated with and predicted better improvement in chronic pain. Resolution of sleep disturbances was more likely to be followed by reports of lower pain intensities. Insomnia was also correlated with disability or limitations to daytime activity. Individuals living with both chronic pain and insomnia were more likely to suffer from mental health issues, such as depression, anxiety, negative mood, suicidal thoughts, and catastrophising (viewing a situation as worse than it actually is). Previously, a literature review found that patients with chronic pain also suffer from depressive symptoms, and that chronic pain negatively affects the recognition and treatment of depression. As depression, pain, and insomnia share similar biological pathways, it is not surprising that these diseases are comorbid with each other.
Treatment options
The most studied pharmacological treatment for patients with fibromyalgia was pregabalin (a medication that is used to treat epilepsy, anxiety, and pain disorders; it exerts an inhibitory modulation of neuronal excitability, reducing the release of neurotransmitters associated with pain). Individuals who received pregabalin showed improvement in chronic pain and insomnia symptoms. Other treatments that showed improvement in both conditions include melatonin, eszopiclone (a sedative-hypnotic used to treat insomnia by binding to GABA receptors) and naproxen (a non-steroidal anti-inflammatory drug to manage acute pain by reducing prostaglandin synthesis).
Cognitive behaviour therapy (CBT) was the most common non-pharmacological treatment that was studied. This is a type of therapy that encourages an alternative way of thinking and behaving to manage an individual’s problem, rooted in the fact that feelings and actions are interconnected. CBT for insomnia was found to improve sleep by decreasing the amount of time taken to fall asleep and increasing the duration of sleep. Reported pain was also mildly improved. For CBT that aims to treat both insomnia and chronic pain simultaneously, the review also found investigations that reported positive treatment for insomnia but no significant improvement for managing chronic pain. Along with CBT, pharmacological interventions, such as pregabalin, can also be administered together and investigated in future studies.
A combination of pharmacological and non-pharmacological treatments is a promising avenue to alleviate the symptoms and co-occurrence of both conditions.
The review conducted by Dr Husak and Dr Bair supports the hypothesis of a bidirectional relationship between chronic pain and insomnia: individuals living with both conditions have a more severe pain experience and longer lasting symptoms, and additional comorbidities, such as mental health problems. The researchers theorised that insomnia could impair essential repair processes during sleep, thereby contributing to lasting development of pain related to dopamine and opioid signalling pathways. Traditional approaches aim to treat insomnia and chronic pain separately, even though the number of individuals with both conditions were found to be high. Moreover, there is limited understanding of the biological relationship between both conditions. Therefore, further studies need to elucidate a concurrent treatment option for individuals with both conditions, so symptoms can be more effectively alleviated for this patient population.

A limitation of this study was that only papers in two databases, OVID Medline and PubMed, were searched for, which may result in some important research not included in this review. A meta-analysis, which combines and measures the statistical significance across various studies, was also not conducted due to the differences in definitions of insomnia, variety of study methodology, and outcomes. A challenge faced by researchers when conducting insomnia investigations is the lack of standardisation across different studies, as the categorisation and diagnosis of insomnia may vary due to differences in subjective and objective sleep quality measures. A variety of methods are utilised when assessing insomnia, such as polysomnography (a test that measures brain waves, blood oxygen levels, breathing, heart rate, and movements of eye and leg), actigraphy (a device worn to monitor sleep cycles), and self-reports. Due to this subjectivity and heterogeneity in methodology, it is difficult to conduct a meta-analysis.
Conclusion
In conclusion, this review emphasises the importance of assessing insomnia and pain in individuals living with chronic pain. A combination of both pharmacological and non-pharmacological treatments is a promising avenue to alleviate the symptoms and co-occurrence of both conditions. It also has the potential to decrease the severity, duration, and comorbidities associated with these conditions, such as mental health problems. Suggested avenues for further investigations include cannabinoids and Internet-based CBT. Moreover, chronic pain is still inadequately treated, which calls for new strategies, such as identifying comorbid conditions and concurrently treating both.
Personal Response
How can individual or group internet-based CBT benefit patients with both chronic pain and insomnia?
Individual or group internet-based CBT can teach useful strategies and skills to patients to better cope with their chronic pain and insomnia. A potential advantage of internet-based CBT is its greater reach to patients that may not have access to clinicians trained to deliver CBT for both chronic pain and insomnia. This is particularly important for patients in rural areas or those with transportation barriers. Patients may also like the convenience offered by Internet-based CBT in that they can access this treatment anytime or anywhere they wish. In the context of the COVID-19 pandemic, Internet-based CBT is especially timely as patients may have increased pain, depression, anxiety, and sleep problems and need help with these conditions, but are fearful to seek medical care in a clinical or hospital setting.