Sinus migraine: A costly blindspot in medical care
Sinus migraine is a frequently overlooked diagnosis and this oversight in clinical care has profound financial and other consequences: a leading misuse of oral antibiotics, inappropriate sinus surgery, and prolonged patient suffering and disability. Although lacking consensus on pathophysiology, diagnostic criteria and nomenclature, medical professionals need to know more about this alternative explanation for patients’ complaints of sinus pressure, pain, nasal congestion, and runny nose. In a review of research, Frederick Godley, MD and his team explore the silent epidemic of misdiagnosed migraines and seek to instil change.
‘Doc, you have to fix my sinuses. I have been on four rounds of antibiotics this year but I keep getting sick.’ When a 55 year old female makes this plea for help, it is easy to assume that the wrong antibiotic has been administered or the patient needs allergy testing or a course of corticosteroids, maybe even some sinus surgery. In a recent literature review published in the American Journal of Otolaryngology, Drs Godley, Casiano, Mehle, and McGeeney lay out an alternative explanation of why patients like this woman do not do as well as we would expect. This patient may be suffering from a form of migraine. Different types of migraine tend to present with different symptoms. One form, sinus migraine, could involve symptoms – facial pain or pressure alongside nasal congestion or a runny nose – which are likely to result in mistaking a sensory nerve malfunction for an infection.

Essentially, they argue that most patients and their caretakers are being fooled by a faulty, or hypersensitive, nervous system, otherwise known as a migraine. Even though clinicians are taught to ask what a patient means when they say they have sinus problems, they often neglect to ask all the questions that might identify a non-infectious cause. Many patients are thus misdiagnosed and receive inappropriate treatment. The review explored the impact of misdiagnosis or delayed diagnosis and found that patients suffer a range of unfortunate consequences including overuse of antibiotics, the cost and risk of sinus surgery and prolonged suffering.
The current guidelines for medical professionals are that the combination of symptoms – facial pain or pressure alongside nasal congestion or a runny nose – is sufficient evidence to diagnose this patient with a possible bacterial infection of the paranasal sinuses and prescribe an oral antibiotic. It is only after the need to use two courses of oral antibiotics that medical professionals are recommended to look “inside” the paranasal sinuses with a CT scan. Moreover, the article points out that most CT findings of the sinuses correlate poorly with the complaints of the patient. Often, normal appearing paranasal sinuses on CT scan can support the suspicion that a patient is experiencing a migraine “sinusitis” mirage.
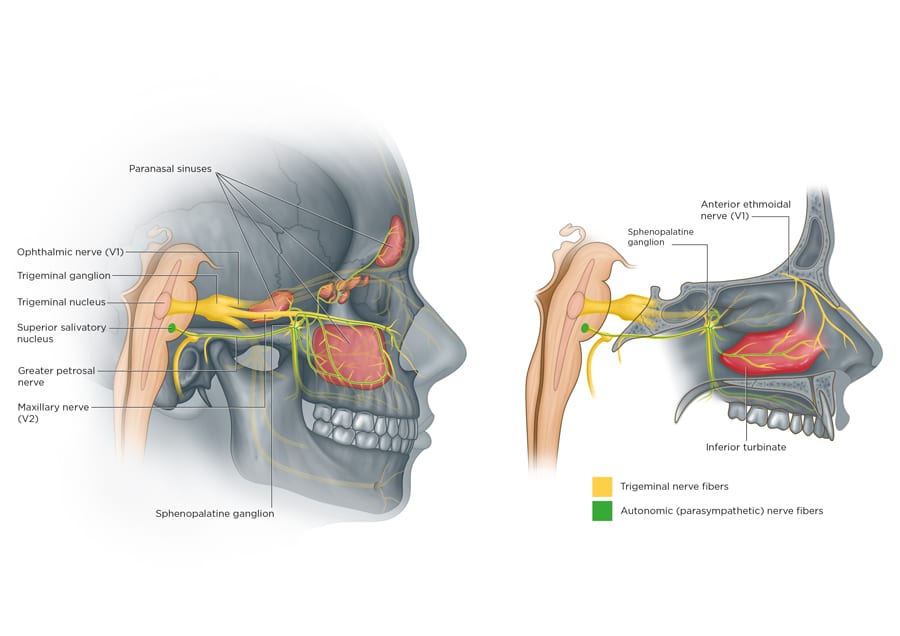
Credit: Francesca Corra francescacorra.com
‘What’s wrong with me, doc?’ – Identifying the cause
While most think of migraine as a ‘nasty’ headache, it is really a disease of the entire nervous system. But what is wrong with the nervous system? Although the specifics have yet to be determined, migraine is a complex genetic condition. There appear to be many genes that, in different combinations, render the nervous system overly sensitive to a stimulus, such as stress, odours, and certain food ingredients.
While most think of migraine as a ‘nasty’ headache, it is really a disease of the entire nervous system.
The authors then speculate how, under the influence of repeated episodes of neuroinflammation and changes in hormone levels, migraine can evolve into a form of chronic sensitisation, or upregulation, similar to allodynia or vestibular migraine. For a patient this might be imagined as a smouldering fire in the brain. In this case, the chronic uncontrolled neural activity involves the second branch of the trigeminal nerve and the autonomic nervous system. It is reasonable to expect the second branch of the trigeminal nerve, which innervates the lining of the paranasal sinuses, to generate pain or pressure in the way the first branch causes headache pain. By the same token, chronic sensitisation can affect the autonomic system, causing dilated vessels and swelling of the inferior turbinates, nasal congestion, and mucus production (runny nose and postnasal drip).

‘How are you going to fix me?’ – Alternative treatment
Only an approach which contradicts current guidelines is likely to recognise correlation between sinus symptoms and migraine. The review article lists a number of clinical studies that show a prevalence of migraine headache, as high as 88%, among those complaining of sinusitis. If medical professionals are to correctly treat a patient presenting with these symptoms it is important that they are sure to consider neurological cause for sinus symptoms.
When rhinosinusitis patients suspected to have migraine disease are treated with migraine medications, the authors cite several studies showing significant (50-80 %) symptom relief.
Meet the team
As the President of the Association of Migraine Disorders, Frederick Godley, MD has used this non-profit organisation to spotlight the broad spectrum of migraine conditions through video podcasts, engage other medical professionals through free online education and accelerate migraine research through a multispecialty coalition of scientists.

As an active participant in research into migraine disorders, Godley understands the importance of building a credible team. His colleagues include Dr Roy Casiano, Professor of the Department of Otolaryngology, University of Miami; Dr Mark Mehle, Assistant Clinical Professor of Northeast Ohio Medical University; Dr Brian McGeeney, Assistant Professor of Neurology from Boston University School of Medicine and Dr Christopher Gottschalk, Assistant Professor of Neurology of the Yale Neuroscience Center. By choosing to combine his own extensive knowledge and personal passion for the subject with the medical expertise of the esteemed co-authors Dr Godley has ensured that their research will have academic impact.
They encourage medical professionals to consider migraine disease as a form of sensory misinformation and as a possible etiology of sinusitis symptoms.
Recommendations and conclusions
The authors identified four key factors which support their theory that a sinus migraine mimics sinus infections. Firstly, current pathophysiology literature offers a model of how migraine attacks could replicate clinical presentations of sinus infections. Secondly, patients with infectious rhinosinusitis and sinus migraine have similar symptomatic presentations and similar demographics, but a sinus CT scan can help to distinguish these two diagnoses when the findings do not correlate well with the symptoms. Thirdly, clinical studies support the proposition that there are alternative diagnostic tools for distinguishing patients with sinus migraine. Finally, some patients diagnosed with sinusitis show significant improvement when they receive migraine treatment.

Until there is a diagnostic test for migraine, clinicians need to question a patient’s self-diagnosis of sinusitis. The authors encourage medical professionals to think of migraine disease as a form of sensory misinformation and as a possible etiology of sinusitis symptoms. Clinicians should ask validated questions to determine if a patient has a history of migraine disease and, if suspected, recommend migraine treatment. Clinicians also may consider examining the paranasal sinuses with a low-radiation cone CT scan earlier in the diagnostic work-up than currently recommended.
The authors would also like to see the promotion of basic science and clinical research that would properly lay the groundwork to teach sinus migraine as a well-established medical diagnosis and change the clinical guidelines to improve patient care.

Looking to the future
As understanding of the risk of antibiotic resistance continues to grow, this research is a well-timed reminder that not only alternative medications, but also alternative diagnosis should be thoroughly explored before antibiotics are used. The team also warn that, under the current guidelines, hundreds of thousands of people may be having inappropriate sinus surgery and other therapies. The authors of the review hope that more research into classifying these symptoms will follow. In the future, this could allow identification of a discrete medical condition- sinus migraine. Ultimately, the most important outcome for all medical professionals is improving patient care and ensuring there is hope for sufferers of earlier diagnosis and quicker access to the best medical care.
Personal Response
Considering the prevalence, are you surprised by the lack of awareness of sinus migraines?
<itemprop=”acceptedAnswer”> No, I am not surprised. This is a fairly new potential diagnosis and one that has not been definitively proven. The pieces of the puzzle are all there and need to be acted on. My personal experience as an ear, nose and throat doctor has anecdotally proven to me that this is a very plausible alternative diagnosis. I have witnessed migraine treatments helping people with sinus issues when traditional sinusitis treatment has not. We now need clinicians and researchers to turn their attention to this very common but deceptive condition.