Thickeners: The evidence for their appropriate use in dysphagia management
Swallowing difficulties (dysphagia), can occur for a number of reasons, including damage to the nervous system, such as a stroke or head injury, or cancer, such as mouth cancer. Dysphagia can be short term, for example while recovering from a stroke, or more long term, for example in dementia or with neurological conditions. There are also different types of dysphagia, depending on which aspect of the swallowing process is affected, and this can result in a range of symptoms. Common symptoms of dysphagia can include dribbling, coughing or choking, pouching or storing food in the mouth, and avoiding mealtimes.Due to the above symptoms, dysphagia has physical and emotional costs to the patient, as well as economic implications for healthcare systems. For example, patients with dysphagia have a 40% increase in length of hospital stay (Altman, Yu & Schaefer, 2010). This means an increase in the cost of their admission and an increased likelihood of experiencing complications secondary to prolonged hospital stay, such as hospital acquired infections. There are also frequent safety concerns relating to dysphagia, such as the risk of aspiration (food or fluid entering the lungs). Patient safety is therefore paramount when managing dysphagia.
The role of Speech and Language Therapists
Dysphagia is usually managed by qualified speech and language therapists (SLTs), allied health professionals who provide treatment and support for adults and children who have difficulties swallowing, communicating or eating and drinking. Early identification of dysphagia is key, and SLTs will use a variety of different techniques to assess swallowing impairment, including bedside screening tools, physical assessment and videofluoroscopy (Steele et al. 2019).
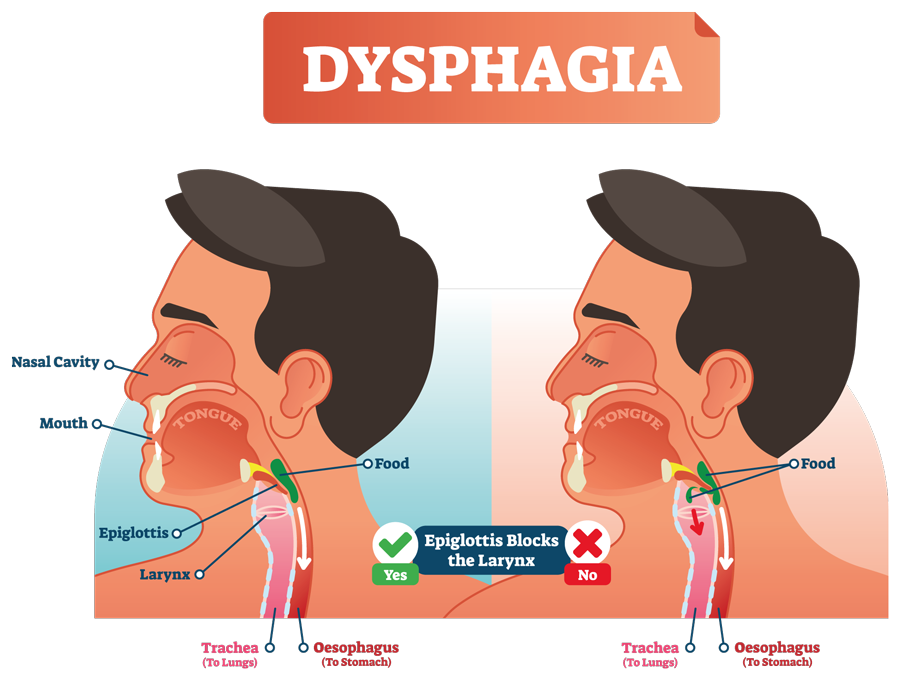
One approach often used by SLTs is the addition of thickening agents to normal fluids to make them more viscous, and therefore easier for patients to swallow.
There are many different thickeners available, including those produced by Nestlé Health Science. As speech and language therapist Sandra Robinson points out, industry innovation can lead to direct patient benefits: the recent move towards using gum-based thickener rather than starch-based thickener ‘was a really useful change for our patients, because it meant that the thickener looked nicer, had an improved taste, and was safer – one of the most important aspects’. In addition to powder-based thickeners which are added to fluids to achieve the correct consistency, it is possible to use ready-made nutritional supplements which are pre-thickened.
While thickeners are widely used, best practice involves using fluids as close to ‘normal’ as possible. Therefore, multidisciplinary working between healthcare professionals is key to ensure that thickeners are used appropriately, especially where there may be a tendency to overthicken (Garcia and Chambers, 2019). Used correctly, thickeners have multiple benefits for dysphagic patients.
Physical impacts
One of the most common concerns with dysphagia is that food or fluids go ‘down the wrong way’, potentially entering the lungs rather than the stomach. If this occurs, the patient is often seen to cough and choke when eating or drinking. There is, though, also a chance they are silently inhaling fluid or food, a situation which could only be identified with special investigations such as a video fluoroscopy of the swallow action.
In acute settings, early identification and management of dysphagia is crucial and can reduce the risk of pneumonia three-fold.
The concern around inhaling food or drink is that aspiration pneumonia may develop as a result. According to Ashford (2005), there are three pillars of pneumonia: health status, oral health status and swallow function. It is the latter where thickened fluids may be beneficial. Thickening liquids is thought to slow the flow rate of the liquid, allowing more time for airway closure and reducing aspiration risk (Cichero, 2013). The aim is to reduce the risk of aspiration pneumonia by reducing the risk of fluid inhalation, thus making eating and drinking much safer for patients, as well as improving their quality of life.
Emotional impacts
Dysphagia can have profound impacts on social and psychological aspects of a patient’s life, particularly when it comes to fear of choking. The latter could even increase risk of malnutrition and dehydration if a patient avoids eating and drinking. There is evidence to suggest that people with severe dysphagia who are worried about drinking thin fluids may appreciate the greater control over aspiration risk that thickened fluids allow (Schindler & Kelly, 2002).
Sandra Robinson recommends thinking about the following values when considering the use of thickened fluids; firstly, the patient’s needs, wishes and preferences, and then how the patient will feel, function and survive if prescribed thickeners. If information is presented to the patient in full, then they can judge the balance between risk and benefit of a modified diet for themselves. Different patients will make different choices depending on their level of concern but for some patients, thickeners can empower them to manage their own health conditions.

Thickeners in practice
While much evidence exists to support the use of thickeners in dysphagia, multiple parties are often involved when it comes to the actual application of thickeners. So, their use requires a consistent, defined approach to ensure that there is interdisciplinary working between SLTs, dietitians, doctors, nursing staff and the patient.
The International Dysphagia Diet Standardisation Initiative (IDDSI) was founded in 2013 to provide consistent and clear terminology around modified textures of food and fluids.
The first step in creating this common taxonomy was to examine the existing data. A systematic review, which summarised 36 high quality studies, was conducted during the creation of the framework (Steele et al, 2015) and the results showed that thicker liquids reduce the risk of aspiration but can increase the risk of post-swallow residue in the pharynx. Where patients feel thickener helps, though, this risk can be managed, for example by encouraging additional swallow movements after each sip.
The IDDSI framework provides professionals with guidance around texture-modified diets. This is especially important when we think about the people who are administering thickener or blending a meal; it is often a busy carer or nurse who requires clear, specific guidance to prepare appropriate food and fluids. As research has shown, there is a place for thickeners in dysphagia, but only if used correctly, monitored, reviewed and used in conjunction with other approaches such as swallowing rehabilitation and use of appropriate drinking vessels (Lippert et al, 2019).
Rather than a one-size-fits-all solution, thickeners are a useful tool as part of a broader approach.
Sandra Robinson agrees with this approach: ‘Thickener can be really useful while a patient also follows therapy, diet adaptation, and undergoes some possible spontaneous recovery from something like stroke. But we should really aim for it to be a temporary measure.’ For some patients, though, she recognises it may be a longer-term solution. ‘It can be a comfort for some people who choke or have prolonged coughing bouts that are thoroughly distressing and uncomfortable, maybe even painful, on regular drinks. In these cases, thickener can reduce the fear of choking, as well as the actual choking, pain and distress, and that might be true of somebody for a significant period of their life or during end-of-life care.’
A holistic approach
Thickeners are a useful tool as part of a broader approach. Foley et al (2008) found that using a combination of texture-modified diet, thickened fluids and intensive support from speech and language therapists resulted in reduced risk of aspiration for the first seven days after a stroke. These results support the use of thickeners in the context of a wider support strategy.

A holistic approach to dysphagia has many benefits: food provides more than just nutrients and plays an important role in the social, emotional and cultural aspects of life. Thickeners, alongside other factors including positioning, use of different eating and drinking vessels, oral hygiene and the possible use of artificial hydration if clinically indicated can be a valuable tool in the treatment of dysphagia. To further the existing knowledge base, clinically meaningful endpoints must be considered when undertaking clinical trials around thickeners, and further research and collaboration between healthcare professionals, patients and other stakeholders is crucial.
Acute and community settings
Julie Cichero, co-chair of the IDDSI framework, reports that in the UK, the annual cost of chest infections requiring hospital admission with routine care is around 1.8 times more expensive than chest infections requiring hospital admission with treatment from a speech and language therapist (Cichero, 2019). Although use of modified texture diets is not specified in this case, it is likely that many of those seen by a speech and language therapist were advised to thicken fluids, suggesting there is an economic benefit to intervention.
Indeed, in acute settings, early identification and management of dysphagia is crucial and can reduce the risk of pneumonia three-fold (Hinchey et al, 2005).
Moving away from an acute setting, care home manager Jemma Robinson feels thickened fluids offer many benefits to her residents, particularly as safety is a priority in this vulnerable population. She says, ‘Thickener means that residents can take their usual fluids, it reduces the risk of aspiration which can cause complications, or it means they do not need to have any other interventions like IV fluids: they can live a normal life.’ It is not only nursing home residents whose lives are impacted; over half of head and neck cancer patients report reduced quality of life due to dysphagia (Garcia-Peris et al, 2007).
Support and training is key
Thickeners and thickened liquids meet the requirements of Food for Special Medical Purposes in the EU (Cichero, 2019), highlighting the need to use thickeners under medical supervision. If thickeners are used incorrectly, they can be unpalatable as well as unsafe. As care home manager Jemma Robinson explains, preparing thickened drinks incorrectly can be just as dangerous as not having the thickener at all. This is where the role of producers in supporting the use of their thickeners is so paramount.
Nestlé Health Science offers support to care homes, other community organisations and individuals with dysphagia, for example through face-to-face or digital safety briefings. Safety underpins their practice and they are dedicated to providing guidance, training and access to relevant services. This is crucial to changing the culture around the use of thickeners, ensuring that it is not seen as the easy option, but is delivered by qualified professionals who understand the influence that thickener can have on gastric emptying times and other variables. In addition, there are clear benefits to using just one thickener within a local area, as this means that everyone is fully safety trained and competent with one particular product, removing the need for multiple pathways and safety briefings for different products.
Overall, there is a role for thickener in managing dysphagia for patients in acute and community settings, whilst being used safely and effectively. Multidisciplinary working is key, as is the use of a holistic approach which uses other strategies to improve health and well-being for dysphagic individuals.
Personal Response
How important do you think collaboration with industry is to the speech therapy profession?
I think for the speech therapy profession working with industry is highly necessary. I don’t think we can get results without each other. There’s the trinity of industry, research and the profession on the ground as well, of course, as patient groups and patient feedback. It’s really important that we’re working ever more closely together.
I think it takes industry to innovate and take things forward, because most of the SLT profession work in the NHS. The NHS moves at a very, very slow pace, as do a lot of higher education institutes. Research takes time and it’s companies like Nestlé Health Science who can really help bring things along and say to the profession, “Look, this is what we can deliver. This is something we’ve developed. How can we bring that ultimately to the patient’s benefit, sooner rather than later?
What do you value most about your role?
I think ultimately, the greatest satisfaction for me is in seeing benefit to patients. It’s the whole point. Knowing that patients have improved after a job well done – you get personal satisfaction from that and the positive feedback from patients. Do you know what? I’ll take negative feedback. I’m happy to have that, just as I’m happy to unlearn. Whether it’s a patient or a peer, I’m happy to question and learn new things.
I think, as a profession, we need to be more open to that and to be saying, “Yes, we will unlearn some of the old ways”. Just as we’ve noticed that industry has moved on, let’s also move on. Let’s find new ways of working together and help give patients exactly what they want.