COVID-19: An individualized treatment framework
The elderly are among those at greatest risk of serious infection and death from the coronavirus (COVID-19). By individualizing treatment for COVID-19 and its complications, a significant advance in medicine and improving care could be achieved. Dr Richard Aguilar and colleagues have developed the first known evidence-based recommendations for individualized treatment. These recommendations were derived from a preliminary review of existing research, followed by implementation of a disease progression and treatment model from a cohort of nearly 40,000 patients. The key to improving outcomes is determining risk and individualizing care. The tailoring of COVID-19 management is in its nascent form.
Coronavirus (COVID-19) presents a dire threat to health, and is an immediate challenge to healthcare. It stands to fundamentally alter several key aspects of the way in which we do medicine. The virus was first reported in China in late 2019 and then rapidly spread around the world. On the 11th of March 2020, the World Health Organization declared a global pandemic. COVID-19 caused more than 2 million deaths within the first year of the pandemic. As a result, researchers, clinicians, and most healthcare organizations mobilized to better understand the virus, develop vaccines, and optimize care.

A significant advance in the effectiveness of medical care and improving clinical outcomes would be achieved by individualizing treatment of COVID-19 and its complications. Dr Richard Aguilar is the Chief Clinical Officer of Cano Health, a primary care healthcare organization which manages >100k lives across Florida, Texas, Nevada, California and Puerto Rico. Dr Aguilar and his colleagues published their evidence-based recommendations for individualized treatment of COVID-19 and subsequently reported on its application in a primary care setting. They demonstrated a significant reduction in hospitalization and mortality from COVID-19 on their patient base. The team have been contributing to these efforts with their large cohort of primarily elderly patients through the implementation and evaluation of individualized care protocols. This was done across their clinics, and included those patients at greatest risk of severe complications.
The work by Aguilar and his colleagues presents the first evidence-based recommendations for individualized treatment for COVID-19.
Early during the COVID-19 pandemic, the team applied their clinical and population health tools to attempt to bend the curve and improve clinical outcomes. Their initial publication in October 2020, Current Understanding of COVID-19 Clinical Course and Investigational Treatments, proposed a treatment algorithm for patients infected with COVID-19. They put forth the concept that a treatment algorithm should be dependent on varying factors such as age, gender, comorbidities, and symptom severity (Figure 1).
After applying these treatment principles to over 38,000 of their Medicare Advantage lives in South Florida, they published their findings, Managed Care COVID-19 Outcomes in a Population Health Program, comparing their results to an age- and gender-matched mirror population in Florida (SOF).

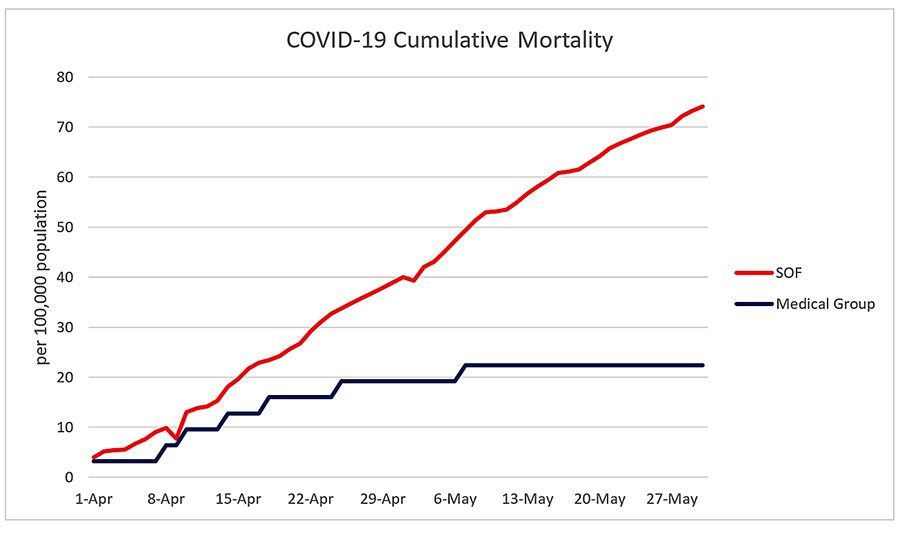
Their findings supported their hypothesis that managed care patients would fare better than a comparable population primarily due to their model of care. This model of care proactively focused on keeping patients healthy rather than being reactionary and just treating disease. Their papers concluded that although the incidence of infection and hospitalization rates for COVID-19 were similar in their medical group compared to the matched Florida population (65+), the mortality was 60% lower for all COVID-19 patients (p < 0.05), and 63% lower for those who were hospitalized (p < 0.05) (Figure 2). Furthermore, they proposed that the introduction of their COVID-19 specific Population Health Program (PHP) was highly correlated to mortality reduction (r= 0.93, p < 0.001). The team believes that the improved outcomes were primarily due to two factors. First, an increase in patient engagement in the form of clinical encounters, home visits, and other direct communication. Second, the optimization of medical management through evidenced based treatment of chronic conditions. These findings were an extension of their stellar improvements across a range of other clinical outcomes for the elderly by virtue of individualized care. Their evidenced-based process rapidly grew Cano Health from a single clinic to >70 primary care facilities staffed by >175 clinicians in four years.
Poor prognosis
Risk factors for poor prognosis from COVID-19 include old age and pre-existing conditions including diabetes, obesity, hypertension, congestive heart failure, kidney dysfunction and chronic lung disease.
Stages of COVID-19
The clinical course of COVID-19 infection described by Siddiqi and Mehra (2020) consists of three clinical stages:
Stage I (Beginning of infection) – Following an average incubation period of 5 days, most symptomatic COVID-19 patients experience mild symptoms such as fever, cough, fatigue, and body aches. These early symptoms usually last 5-7 days. During this time, the virus multiplies and becomes established in the respiratory tract of the host. Severity of symptoms in Stage I correlate with the peak viral load.
Stage II (Pulmonary involvement) – Some patients progress to Stage II of the virus. Stage II is characterized by a decrease in viral levels and an increase in localized inflammation within the lungs. A computerized tomography (CT) scan or chest x-ray would show infiltrates (airspaces that become filled with other bodily cells or fluids) in the lungs and give the appearance of increased soft tissue density. This stage lasts for a similar length of time as Stage I (5-7 days).
Stage III (Systemic inflammation) – Only a small percentage of patients (10-15%) progress to Stage III. This stage is associated with inflammation throughout the body (extra-pulmonary systemic hyperinflammation syndrome). Unfortunately, the prognosis and recovery from Stage III is poor. Mortality is around 20-30%.
To maximize the likelihood of recovery from COVID-19 infection, it is important to rapidly recognize the stage at which the patient is ill and treat them accordingly. However, as this is a new virus, no treatment framework has been developed or standardized.
Review of existing research
In April 2020, Dr Aguilar and his colleagues from Cano Health began to tackle this new challenge in care. In order to implement an individualized care process across their clinics, they derived the first evidence-based recommendation of individualized treatment from existing COVID-19 reports. These are essential, given the variability of patient clinical presentation and survivability.
A literature search was conducted to find all relevant studies related to COVID-19. The search dates were bracketed between the dates April 1 to April 13, 2020, using the following electronic databases: PubMed (1809 to present); Google Scholar (1900 to present); MEDLINE (1946 to present), CINAHL (1937 to present); and Embase (1980 to present). Aguilar and his colleagues located and reviewed 70 relevant studies on COVID-19 that were stored in medical and scientific databases. Their recommendations also drew upon guidelines from hospitals and clinics instructing their staff on procedures to follow. In addition, some decisions were based on data collected by organizations including the CDC, FDA, IHME, IDSA, and Worldometer. The largest group of participants numbered over 500 and some case studies had fewer than 30 patients.
The researchers focused on the following aspects of COVID-19 management: staged progression, clinical algorithms and individualized treatment. Based on their systematic review, Aguilar and colleagues created a model for the clinical stages of COVID-19, diagnostic tests, disease management and treatment options. The results focused on providing individual treatment recommendations by matching the most appropriate drug or treatment action for a given patient. For some patients, the treatment algorithm finds that no treatment is warranted; for others, treatments were based on age, pre-existing conditions, and severity of COVID-19 symptoms.
Individualized treatment
In Cano Health’s model, disease progression was related to the level of infection, extent of inflammation and survivability of the patient. The individualized treatment plan for COVID-19 first considers age and pre-existing medical conditions. Second, the severity of COVID-19 symptoms and stage of infection. It also includes a provision to update the treatment plan as patients progress through the stages of COVID-19 infection.

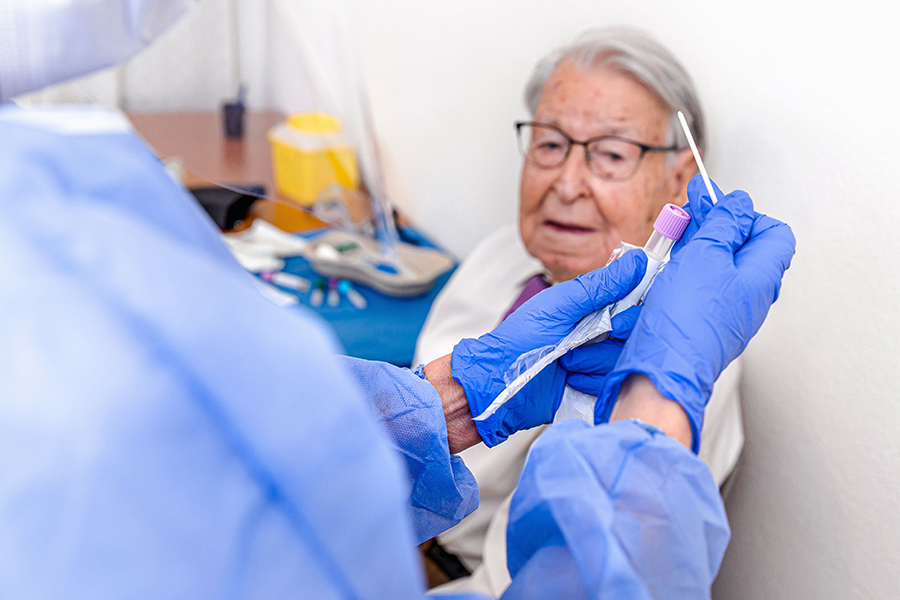
Stage I – During Stage I, the appropriate diagnostic test is a nasopharyngeal (nose/throat) swab. Symptoms are usually mild and viral load is high in this stage. The appropriate treatment is generally supportive care or antiviral medication. Treatment must still be individualized based on age and pre-existing health conditions.
Stage II – There is a decline in viral load during Stage II, so treatment with antiviral medication is less effective than Stage I. Stage II can be divided into two substages (IIA and IIB) depending on the oxygen levels in the patient’s blood. Patients in Stage IIB are described as hypoxemic (with abnormally low levels of blood oxygen). Patients in Stage IIA are not hypoxemic and have normal levels of blood oxygen. The distinction between Stage IIA and IIB is important: in Stage IIB, the patient is likely to have difficulty breathing and corticosteroids (e.g., dexamethasone) may be considered. Oxygen supplementation care is given if needed, or anti-inflammatory treatments (e.g., colchicine). The use of these medications depends on age and pre-existing health conditions.
Stage III – In Stage III, the most important symptom is respiratory distress. Patients may have shortness of breath, rapid breathing, and have a bluish tinge to their skin. Treatment may include antiviral medication in the presence of a high viral load. Anti-inflammatory drugs and anti-coagulants medications should be considered.

Some clinical trials have also explored pre-exposure and post-exposure prophylaxis (preventative antiviral treatment), but these approaches await more definitive research on their efficacy.
Evidence-based treatment in practice
The results of their literature review emphasized the patient treatment options to their baseline level of risk along with their stage of COVID-19 infection. Clinicians at Cano Health put this into practice to improve COVID-19 outcomes among their predominantly elderly Latino patients, many of whom have one or more pre-existing health conditions.
Dr Aguilar’s group conducted a retrospective cohort study comparing managed care patients with an age- and gender-matched mirror group from April 1, 2020 to May 31, 2020. They identified high-risk patients by compiling medical records, pharmacy use, hospital admission history and other medical statistics from their electronic medical records (EMR) platforms, which readily provide detailed case data for analyses. A total of 38,193 patients at high-risk for COVID-19 were monitored for clinical outcomes including COVID-19 incidence, hospitalization and mortality. The PHP involved contacting patients regularly and patients who declared symptoms of COVID-19 were immediately tested and enrolled into the individualized treatment plan. Within Cano Health clinics, the highest risk patients (those diagnosed with COVID-19 or at high risk for COVID-19) were managed by the Medical Group’s COVID Task Force (CTF), which contacted patients, conducted medical encounters, and tracked data including comorbidities, treatment response and medical outcomes. This protocol was accepted for publication, Managed Care COVID-19 Outcomes in a Population Health Program, Am J Manag Care 2021; Vol.27(6) p.294-300: In Press. Feb 2021.

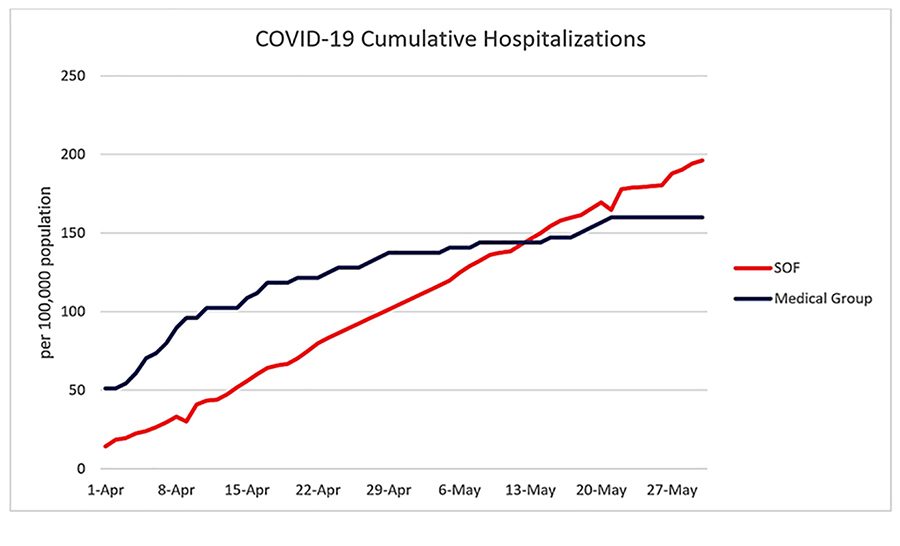
By implementing the Medical Group’s COVID-19 PHP, patients were diagnosed and treated early for COVID-19 and/or underlying disease using a proprietary COVID-19 survey. The COVID-19 survey was designed by the Medical Group’s physician leadership, with specialty certifications in Internal Medicine and Family Medicine. The survey scores ranged from 0 to 162 based on age, pre-existing comorbidities, current symptoms, length of illness, testing and diagnostic status for COVID-19, infection status of household members, current treatment, availability of medications (to treat chronic, underlying medical conditions), and experience using Telemedicine. Patients were then sorted into one of four risk groups based on the score: low (0-10), medium (11-29), high (30-40), and very high risk (≥41). Patients with a score ≥30 or who were positive for COVID-19 were assigned to the COVID-19 CTF. The CTF was a team of clinicians and other healthcare professionals assigned to manage patients. The CTF utilized a COVID-19 treatment protocol developed by the Cano Health’s clinical team, based on the findings of their previous study. The patient’s health status was continually monitored and updated, and treatment of underlying comorbidities optimized. The mean age of the Medical Group’s samples was 67.9 years ± 15.2 years, 61% female and 39% male. Among their managed care patients, older age and hypertension were the most important factors predicting COVID-19. Obesity, chronic kidney disease, and congestive heart failure were linked to higher rates of hospitalizations. After the initiation of COVID-19 surveys (as part of the PHP) on April 6, the incidence of COVID-19 related hospitalization for patients in the Medical Group declined significantly by 63% (49% vs 28%, p less than 0.05) (Figure 3). They also reported a significantly reduced risk in mortality 60% (9.1% vs 1.6%, p less than 0.05) compared to the mirror group leading them to propose that individualized proactive care was strongly associated with improved outcomes in Cano Health’s large high-risk patient population.
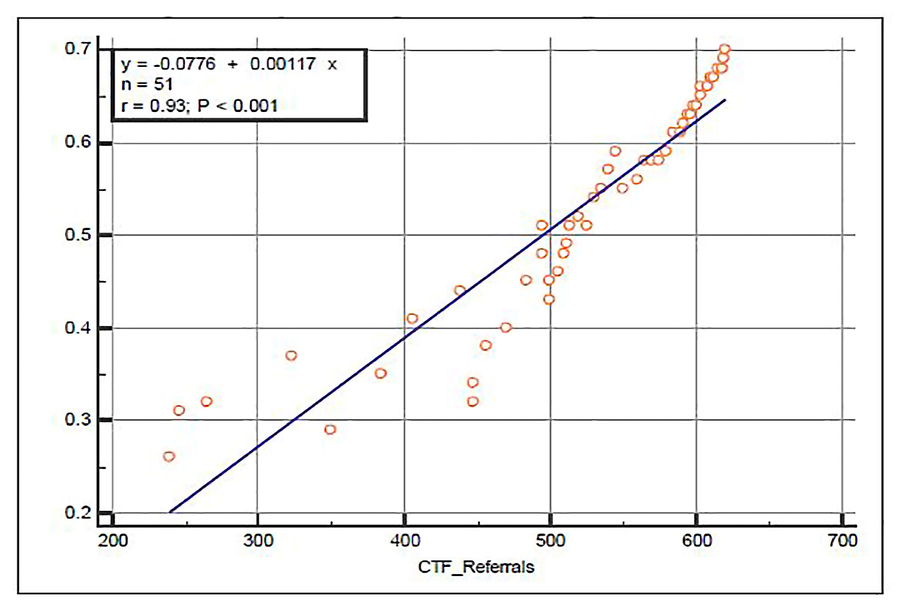
A correlation was found between CTF referrals and overall mortality reduction between the Medical Group and the Florida mirror group over time (r = 0.93, p < 0.001) (Figure 4). The mortality reduction was found to be significant after controlling for age, gender, outpatient treatment, and all studied comorbidities. In addition, they put forth the idea that the introduction of their COVID-19 specific PHP was highly correlated to mortality reduction (r = 0.93, p < 0.001).
In Cano Health’s model, disease progression was related to the level of infection, extent of inflammation and survivability of the patient.
The work by Aguilar and his colleagues presents the first evidence-based recommendations for individualized treatment for COVID-19. Their reduced hospitalization and mortality data was published by the American Journal of Managed Care. These findings are limited by the flux of recommendations as the medical community learns more about COVID-19, and this data is a large stride in the right direction.
Their results suggest that a comprehensive PHP within the context of managed care, in which highest risk patients are identified and treated early, may significantly reduce mortality from COVID-19. This was true for their senior population, as compared to age and gender Florida matched controls. Although they used several off-label treatments, this study was not powered to evaluate the effect of any particular treatment modality. Moreover, their program also included several additional outpatient interventions, such as the delivery of pulse oximeters and oxygen concentrators to the patient’s home. This outpatient intervention may have provided additional clinical benefit through selection of therapy and setting of care.
This data suggests that the delivery of a proactive patient centered approach to primary care can lead to significant improvements in healthcare outcomes, especially in the underserved population. In addition, their study adds to a growing body of work concluding that the delivery of healthcare services that is removed from episodic care to directed pre-emptive care can result in significant benefits. This narrative is especially critical in low socioeconomic circumstances, where morbidity and mortality tend to be higher and where access to care is a major barrier to improving health outcomes. COVID-19 has presented a monumental challenge to our healthcare system and the high incidence and complexity of this disease requires a paradigm shift in our healthcare delivery from reactive to a targeted proactive approach. This approach should be led by primary care providers who work on the front line in conjunction with targeted state of the art population health data and the implementation of optimized standards of care management for chronic diseases.
Personal Response
What is the next priority in COVID-19 research?
Managing patients during the post COVID-19 infection period. Especially those with lingering symptoms of pulmonary compromise (continued use of oxygen and shortness of breath) and mental complications which may lead to prolonged confusion and lack of concentration (i.e. poor lung function and cognitive declines).
What are the best tools for following these patients?
Incentive spirometry metrics, such as: how to manage patients with low Fi02, use of inhaled steroids CT scans, neuropsychiatric evaluation/treatment, etc. Tracking the longevity of the resulting immunity as well as possible re-infection rates that we are now seeing and being reported. Dealing with the possibility of yearly COVID-19 vaccinations, the emergence of COVID-19 variants and the establishment of standardized outpatient treatment regimens. Early treatment intervention to reduce the inflammatory complications resulting from the cytokine storm eventually leading to blood clotting disorders, respiratory distress and multi-organ damage.
Are there similar treatment frameworks for other conditions?
There are other diseases that result from an overactive immune response, such as the autoimmune inflammatory diseases. Interestingly, steroids and hydroxychloroquine are used (or have been proposed) for the treatment of both COVID-19 infection and rheumatologic autoimmune disorders. Commenting on rheumatologic disorders in children, Dr Randy Cron, a pediatric rheumatologist and immunologist at the University of Alabama at Birmingham and co-editor of the 2019 textbook Cytokine Storm Syndrome: “They tend to be sicker than you expect.” https://www.bbc.com/future/article/20200505-cytokine-storms-when-the-body-attacks-itself
Early evidence, again from China, indicates that the antibody tocilizumab (Actemra) may be beneficial for COVID-19. This antibody clogs the IL-6 receptor and inflammatory cytokine, preventing cells from receiving the IL-6 message. Tocilizumab is normally used to treat arthritis and to alleviate cytokine storms in cancer patients receiving immunotherapy.