Time for a new approach to severe traumatic brain injury and stroke: Developments in automated, real-time monitoring of brain stem function
The human brain is an electrophysiological marvel. By the virtue of ionic chemical gradients creating minute electronic pulses, about 80 billion nerve cells have set up an electrical grid with 20 Watts of power. Although just enough to illuminate a small light bulb, the complexity of the brain is far and away unequalled by any man-made system and will likely remain so. Beginning with the first man-like creature, 4-5 million years of evolutionary shaping and adaptation has led the human brain to a complexity only partially mirrored on earth by our primate ancestors. The durability of the human brain to maintain high level, sophisticated functioning for a lifetime, under many manners of perturbation, speaks to a majestic beauty of design and architecture.
Brain malfunction due to head trauma or stroke (insufficient blood flow to the brain) resulting in death or disability is not an infrequent occurrence. Indeed, stroke is the world’s second most frequent cause of death (about 6.3 million deaths per year, World Health Organization, 2016).
When both mortality and permanent disability are factored in, Traumatic Brain Injury (TBI) is estimated to affect 50 million people each year. Although receiving more attention recently, TBI has been a major but largely neglected global problem. It is the leading cause of mortality in young adults, a major cause of disability across all ages, and believed to increase the risk of late-life dementia. Financial consequences of TBI are estimated to cost the global economy $400 billion annually (Maas et al, Lancet Neurol 2017;16:987-1048).
Current approaches and limitations A non-invasive, real-time, automated and alarmed warning system is necessary to capture the earliest signs of TTH – allowing adequate time for physicians and surgeons to intervene. In this setting TTH is a frequent cause of fatality or severe disability, as bruising and damage develops in the midbrain portion of the brainstem or adjacent regions. Onset of TTH is usually associated with changes in pupil size or reactivity and complicates severe TBI in about 30–40% of cases. Deterioration leading to TTH may also be seen in up to 20% with moderate TBI, large volume stroke, or other brain conditions. Pupillary changes with TTH can occur within minutes or several hours or days after injury. Once present, TTH is not always fully reversible following urgent neurosurgical decompression. A non-invasive, real-time, automated and alarmed warning system is necessary to capture the earliest signs of TTH and allow adequate time for physicians and surgeons to intervene. In many other cases haematoma size, brain swelling and midline shift are not deemed significant to warrant surgery, and the patient is observed in an intensive care unit (ICU). Once or twice per day the sedation can be temporarily withdrawn in a cursory and often unreliable effort to examine the patient’s ability to respond to pain stimuli and move extremities. Unfortunately, many patients under observation deteriorate several days later, and without apparent warning slip into various degrees of TTH. The culprit is often progressive brain swelling or consolidation of cerebral contusions, compounded by respiratory or fluid issues. Over the past 3–4 decades, critical care emphasis for severe TBI has been on placement of an invasive ICP monitor within the ventricles (fluid-filled cavities in the brain) or in the brain tissue itself. Ventricular placement may provide a more accurate pressure and fluid drainage may help control ICP – but only if the ventricles are adequately open and communicate. ICP monitors are routinely placed on the side opposite the major damage, for fear of inciting further damage or deterioration in placement, and thus may underestimate the ICP level, or propensity for TTH. Because the brain is enclosed within the hard, rigid skull one may assume a measurement anywhere within the skull or brain will reveal a global pressure – much like the air pressure in an automobile tire. Unfortunately, this is not so. In fact, the brain tissue itself (about 70% of the contents of the skull) is predominately a viscoelastic (plastic) solid structure and not of liquid composition like the ventricular fluid. Being highly non-compressible yet deformable, the brain substance is prone to develop pressure gradients especially within semi-closed compartments like the temporal and cerebellar cavities. Close to the brainstem, these are not areas for ICP placement. The insidious onset of TTH may thus occur. A non-invasive monitoring device that can capture the early development of TTH, before pupillary changes occur, and lead to prompt medical and/or surgical treatments would greatly decrease the high mortality and very significant permanent disability in those who survive. “Uncontrolled ICP” can be fatal. However, that situation is more often encountered where surgery was not initially required, but Neuro-ICU medical treatments begin to fail. It likely indicates some gradual degree of TTH herniation has begun, even if the pupil size and reactivity have not yet changed. At this desperate point, a surgical decompression or debulking of cerebral contusions or swelling (oedema) may be considered, but lacking a brain function monitor to guide us, timely opportunity often slips away. It must be understood that the brain functions as an electrochemical organ and ICP measurement does not directly relate to any specific brain function: it remains a distinctly indirect measure of brain dysfunction. It should be appreciated that development of non-invasive, robust, continuous, neurophysiological recordings of basic brainstem (midbrain) conductivity/viability is within our reach. It has been proved in controlled experiments in subhuman primates that a significantly earlier warning of TTH comes with such brainstem (midbrain) recordings from the scalp following auditory stimuli compared to ICP recordings. Dr Stone and his team feel the goal should be development of continuous neurophysiological monitoring for the earliest warning of TTH, when the patient’s functions may still be salvaged. Over the past 30 years, general advances in Neuro-Intensive care including the adoption of ICP monitoring have shown clear improvements in the mortality of severe TBI, but significant improvement in the number of survivors with a favourable outcome has not been forthcoming. Recently, a study protocol treating severe TBI patients in the absence of ICP monitoring showed that frequent CT scans, especially when elevated ICP was suspected and treated, in addition to periodic sedation withdrawal clinical examinations, yielded outcomes not significantly different from those randomised to ICP monitor-based protocols. The authors warn that the above protocol warrants further study, but “the evidence suggests the absence of ICP monitoring does not preclude obtaining satisfactory recovery through aggressive management without such monitoring.” (Chestnut, et al J Neurotrauma 35:54-63. 2018). Recovery from brain trauma is a time game, where minutes really do matter. Diagnosis within the first three hours can drastically improve patient outcome. A better way? Whilst at the Cook Country Head Injury lab, Stone used an intracranial balloon within the temporal/parietal skull of monkeys to study increases in ICP and its effect on brain function up to the point of TTH. Vital signs, pupil size and reactivity and Evoked Potential (EP) responses were also recorded. EP responses are a type of neural activity evoked by a particular stimulus. Stone’s work primarily focused on somatosensory evoked potentials (SSEP) and brainstem auditory evoked potentials (BAEP) also known as the auditory brainstem response (ABR). In simple terms, the test for BAEP involves presenting patients with a sound, typically a ‘click’, at various loudness levels and monitoring the neural response from the midbrain portion of the vital brainstem. A strong correlation was found between changes in BAEP, SSEP and increases in ICP as a balloon was inflated gradually over a four-hour period. BAEP gave the most sensitive warning before TTH, signalled by changes in the pupils, followed by the ICP and SSEP. A new standard Future directions Whilst their improvements over other measures are clear, limitations still exist. These measurements at present are by no means automated, requiring a technician to take repeated measurements, as well as later interpretation of results. For Stone, there is a need to develop automated, nurse/staff friendly neurophysiological monitoring with alarms in the Neuro Intensive Care Units to best utilise these vital BAEP measurements (Stone et al 2017). He draws parallels with neurosurgical operating theatres where such monitoring already exists, implemented to alert staff when certain critical thresholds are reached. Such a system would achieve efficient, user-friendly monitoring of brain-trauma and other patients that is cost-efficient and staff-friendly with great potential to enhance both patient survival and outcome quality. His goal is partnership with industry to build a prototype of Coma AlertTM and begin implementation and studies in New York City where he presently resides. Is there any particular metric of success in this field of post brain-trauma monitoring which you think would be easy to frame for the general public?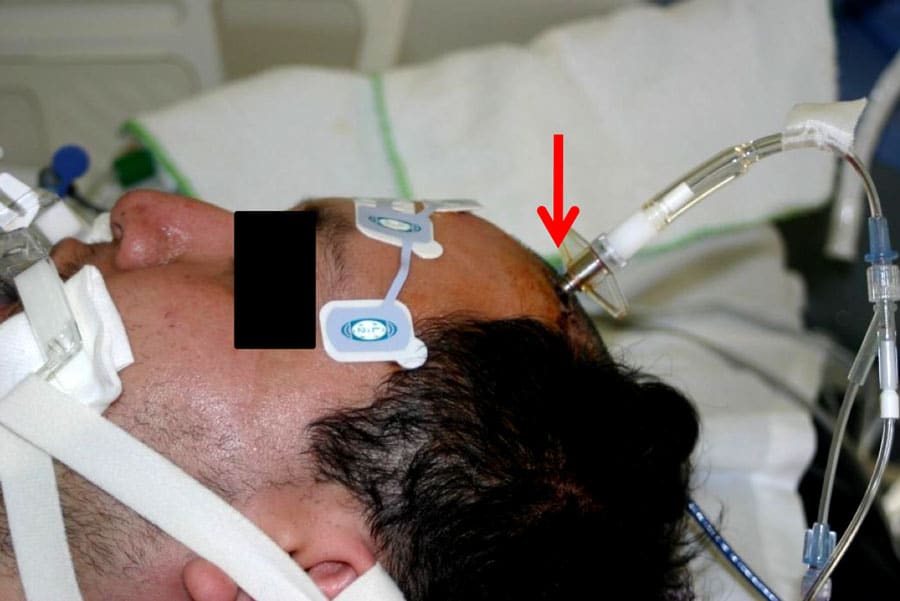
The key to improving outcome after severe TBI, deteriorated cases of moderate TBI, large volume stroke, or any large space-occupying brain condition with altered consciousness demands rapid diagnosis and timely treatment. Prompt airway intubation and adequate ventilation is required to reduce carbon dioxide levels – which lead to both engorgement of the blood vessels in the brain and increased intracranial pressure (ICP). Once intubated, the patient must be sedated. Under sedation, the usual clinical neurological indicators are lost other than the reactivity of the pupils. A CT scan of the brain must be obtained as soon as possible to determine the presence of skull fractures, haemorrhage or contusion within the cerebral tissue, and haematomas (subdural or epidural) compressing the cerebral brain surface. Haematomas or swollen brain tissue may cause concerning midline shift and crowding at the base of the brain, resulting in herniation of the medial temporal lobe. This displaces the midbrain and adjacent deep structures (vital to life) across the midline (known as uncal or transtentorial herniation, TTH).
Dr James Stone has been studying TBI function for over four decades. He has followed every milestone and progression in technology the field has seen. Stone recognised that as an electrical organ, the brain would benefit from more direct and sensitive measures of neural activity. His early sub-human primate work established animal models of ICP and TTH progression and concurrent brain dysfunction monitored by sequential Evoked Potentials (EPs).
From this point onwards, Stone aimed to establish a more sensitive and earlier warning of TTH using the BAEP (Wave V and Vn amplitude and latency measures) examination. At the time, BAEP waves took approximately 7–8 minutes to record; Stone aimed to reduce this delay to 3–4 minutes. To achieve this, he developed modified BAEP (mBAEP) in animals and human volunteers by altering the auditory stimulus used by stimulating both ears simultaneously, increasing the rate of presentation (both build V and Vn amplitude) and utilising four diminishing loudness intensities. Recording electrodes are placed on the forehead and neck. 75 normal hearing human volunteers established appropriate mBAEP testing modalities for study. Next, about 150 patients with cerebral brain lesions were studied in order to test reliability of the mBAEP. A number of patients had concurrent measured ICP values. The standard BAEP at two different sound intensities, as well as the mBAEP was also performed in over 100 patients. In more recent studies, Stone used CT scans and MRI scans of the patients to document the size and locations of the lesions and improvement of mBAEP after surgical removal of the mass lesion. This allowed the use of multiple comparative measures to assess validity and sensitivity. Compared to the standard BAEP, Stone’s mBAEP produced more prominent V and Vn waves for latency and amplitude measurements. This allowed greater and more robust statistical analyses. Importantly, this meant a faster and arguably more reliable measure of midbrain dysfunction than the standard snapshot BAEP techniques currently employed.
As a collective, Stone’s work has sought to highlight the need for improved brain monitoring of severe TBI, large volume stroke, and other space occupying brain lesions and dysfunction at earlier stages than other popular approaches yielded. The introduction and progression of the brainstem auditory evoked potentials (BAEP) continues to be a success in this direction. Across a number of studies, Stone has demonstrated the efficacy of mBAEP.Personal Response