Riding the cardiac wave: The link between incremental pulse wave velocity and cardiovascular risk factors
Cardiovascular disease (CVD) is a major health concern. Arterial stiffening is known to be linked to CVD risk; therefore, establishing effective ways to measure this provides a novel way to screen populations and to detect early signs of CVD. Dr P M Nabeel, Dr Jayaraj Joseph, and Professor Mohanasankar Sivaprakasam at the Healthcare Technology Innovation Centre, Indian Institute of Technology Madras, have investigated the use of a new marker called incremental pulse wave velocity (a measure of arterial wall dynamics) to identify CVD risk employing ARTSENS®, a device for non-invasive, automated evaluation of arterial stiffness.
Cardiovascular diseases (CVDs) are conditions that affect the heart and blood vessels, and deaths associated with CVD are usually caused by heart attacks, heart failure, or strokes. CVD is the leading cause of death worldwide, accounting for around 18 million deaths each year.
There are many factors that influence CVD risk, including genetic, environmental, and lifestyle factors. One factor associated with increased risk of cardiovascular events is arterial stiffness. Arterial stiffness describes a process which can occur as a result of ageing and arteriosclerosis (the thickening and hardening of artery walls). This can impact blood flow, for example by restricting the amount of blood that reaches tissues of the body. As a result, the heart has to work harder to push blood round the body, and this increased workload can damage the heart.
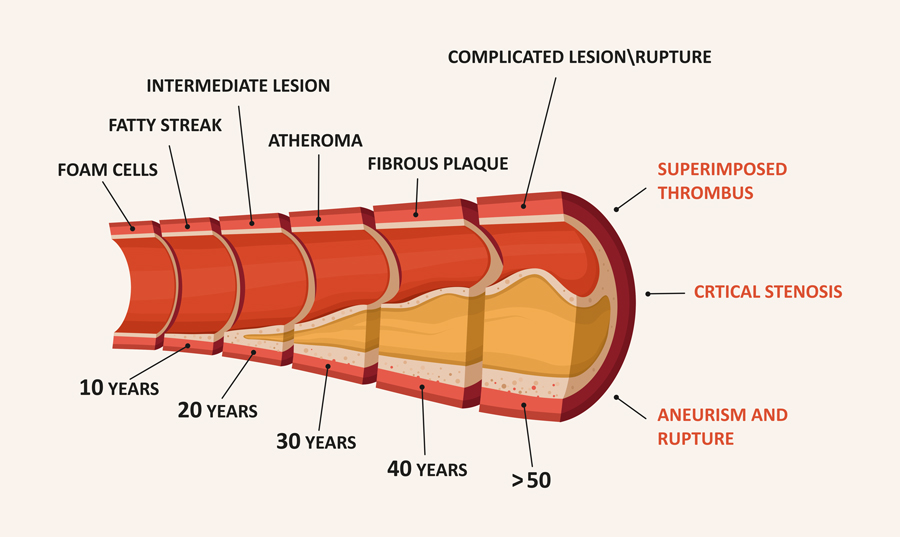
Arteriosclerosis can also be caused by the build-up of fatty plaques and cholesterol on the artery walls, something that is impacted by both lifestyle and genetic factors, such as diet, smoking, and physical activity level.
What is ARTSENS®?
Due to the link between increased risk of CVD and increased stiffness of arteries, particularly in the carotid arteries (the main blood vessels that carry blood to the brain), non-invasive measurements of arterial stiffness offers a promising option for screening and early detection of CVD risk. Existing devices for measuring arterial stiffness are often expensive, require expert operation, and cannot be used in everyday clinical settings. This highlights the need for alternative, easy-to-use methods to measure arterial stiffness.
Non-invasive measurements of arterial stiffness offer a promising option for screening and early detection of CVD risk.
Dr Jayaraj Joseph, Professor Mohanasankar Sivaprakasam, and Dr P M Nabeel at the Indian Institute of Technology Madras, Healthcare Technology Innovation Centre, have developed ARTSENS® (www.artsens.tech), a device that can be used for non-invasive, automated evaluation of arterial stiffness. ARTSENS® uses single-element ultrasound to obtain information about the carotid artery, which is then fed into algorithms that can extract arterial measurements and translate the data into clinically recognised measures of arterial stiffness.
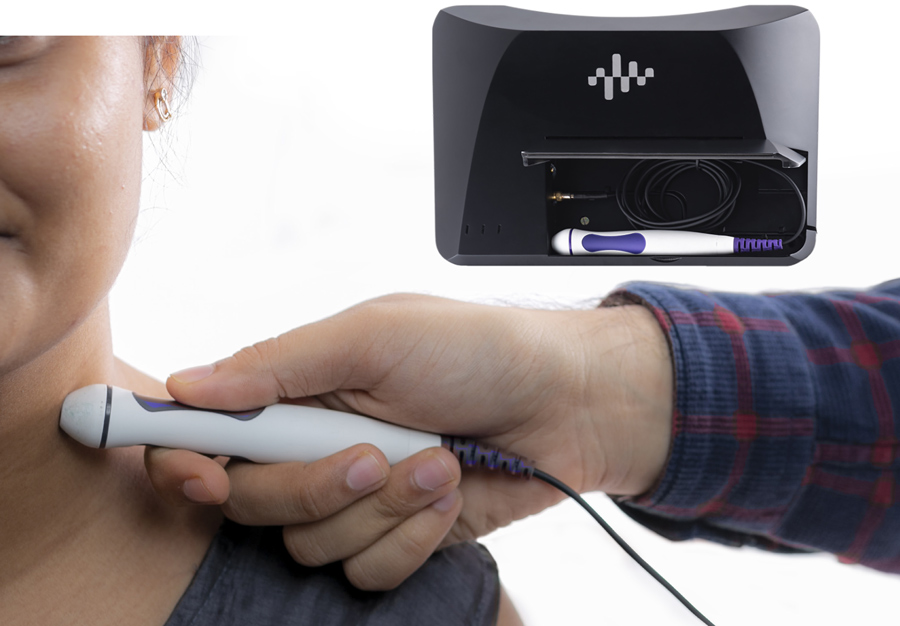
So far, the researchers have created two ergonomic versions of ARTSENS® to take multiple measurements of cardiovascular health. The ARTSENS® Pen offers a novel solution for large-scale screening and population studies. It is a portable device that is able to rapidly assess carotid artery stiffness. Firstly, the patient’s blood pressure is measured and entered into the device. An image-free ultrasound probe is then placed over the neck at the carotid artery location to evaluate the geometrical and material properties of the artery wall. The device is then able to calculate the degree of arterial stiffness.
For a more thorough vascular health assessment, the team has developed ARTSENS® Plus, a device that is able to measure carotid artery stiffness, but which also considers aortic pulse wave velocity (a way to measure the stiffness of the main artery from the heart) and blood pressure from different arteries of the body. This device can be used in both research and clinical settings to pick up early indications of vascular ageing and CVD.
Both devices use intelligent algorithms to automate measurements, removing the need for complex instructions, and reducing the variety that can occur when different people measure the same target. The technology has already been field-tested on over 5,000 subjects and offers a solution to large-scale screening for cardiovascular risk.
A new vascular health marker
Nabeel, Joseph and Sivaprakasam have also proposed a novel way in which vascular health can be measured using incremental pulse wave velocity (ΔC). Every time the heart beats, it generates a pulse, or wave, that travels through the circulatory system, pushing blood around the body. ΔC measures how much the speed of the blood pulse changes within each beat of the heart, at the arterial site under investigation. This means that it is able to provide information about how elastic the walls of the arteries are, as well as other aspects of arterial wall dynamics.
Arterial stiffness means that more effort is needed for blood to pass through the vessels, as elastic arteries would normally buffer pulsatile blood flow and ensure an even flow. Putting more force on blood flow can thereby lead to an increase in blood pressure.
Previous studies have shown that pulse wave velocity from the aorta, the main artery that carries blood from the heart to the rest of the body, can be a useful predictor of cardiovascular illness in several populations, including individuals with kidney disease, diabetes, or high blood pressure. However, ΔC is not currently used as a routine clinical tool.

Pulse wave velocity can be measured by calculating the time that is takes for an arterial pulse (resulting from a beat of the heart) to move between two specified points in the body. Generally, this tends to be between the carotid artery in the neck and the femoral artery in the thigh.
The researchers’ study is the first and largest population trial to explore ΔC. Previous barriers have included a lack of a non-direct and effective method for evaluating ΔC in a clinical setting as well as the absence of a cost-effective tool that is appropriate for use in field studies. The team carried out a cross-sectional study, meaning that they looked at data from a population at a specific time point. They measured ΔC in the carotid artery for 1,373 participants using ARTSENS®.
Early detection of cardiometabolic abnormalities
While previous work has explored the link between pulse wave velocity and CVD, no work has been done to understand the links between ΔC and cardiometabolic abnormalities, such as those seen in metabolic syndrome. Therefore, the research team also characterised risk factors for metabolic syndrome in the participants. They found that 403 of the participants did have metabolic syndrome, a term used for a combination of diabetes, high blood pressure, dyslipidaemia and obesity, which can increase risk of CVD.

The results of the study showed that there was a positive association between ΔC and cardiometabolic risk factors. ΔC was around 28% higher in individuals with metabolic syndrome compared to those without risk factors. The researchers also found that ΔC increased when the number of risk factors for an individual increased. The risk factors considered in this study included elevated blood-sugar levels, high cholesterol, high blood pressure, and obesity. In particular, high blood pressure showed the largest impact on ΔC.
Incremental pulse wave velocity was around 28% higher in individuals with metabolic syndrome compared to those without risk factors.
Interestingly, women with metabolic syndrome tended to have higher ΔC than men with metabolic syndrome. This is likely to be due to gender-specific molecular mechanisms and highlights the importance of considering different clinical diagnostic and treatment pathways for different genders.
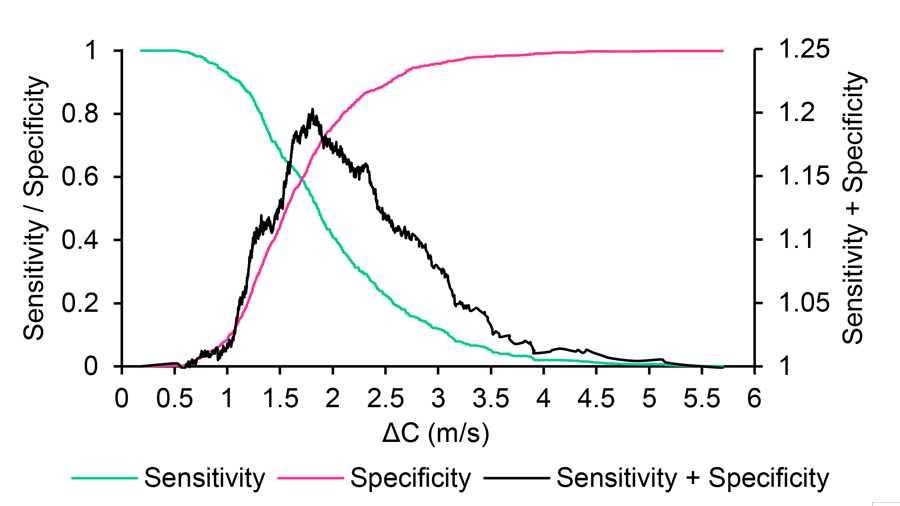
In addition, the study showed that ΔC may be able to predict the number of complications relating to CVD and metabolic syndrome at a population level and was able to achieve this more accurately than methods that are currently used. For example, a ΔC >1.81m/s would suggest that an individual had three or more risk factors relating to metabolic syndrome. In addition, risk analysis suggested that these individuals were also 1.7 times more likely to develop cardiometabolic complications than those with ΔC <1.81m/s.
ΔC was able to detect very small changes in arterial dynamics that occur with certain risk factors for CVD or with other metabolic alterations. The researchers explain that using ΔC in routine vascular health screening may therefore offer more accurate and relevant information than conventional screening methods.
Using ARTSENS® devices for the early detection and screening of vascular abnormalities not only improves identification of patients who may be at risk of developing complications but also offers a possible tool that can be used in both clinical and epidemiological studies to expand understanding of vascular health.
Early assessment of vascular markers allows treatment strategies to be optimised and provides a window in which preventative strategies could be applied to reduce the risk of CVD complications. There is also an opportunity to establish cut-off values of ΔC that could be used for CVD risk stratification at a population level.

Personal Response
What are the next steps to encourage routine use of incremental pulse wave velocity for CVD screening?
Incremental pulse wave velocity – ΔC – describes vascular structural and functional alterations and demonstrated a positive association with cardiometabolic risk factors. Our study provides evidence for the use of ΔC for early detection and screening of vascular dysfunction. Assessment of ΔC in clinical practice can provide pathophysiological particulars that are not currently captured by conventional vascular markers. We have developed and validated a fully automated image-free ultrasound device for rapid and easy assessment of ΔC in clinical settings, which is currently deployed at multiple sites. Availability of such easy-to-use devices and large-scale clinical studies for establishing the efficacy of such assessments are key to the widespread adoption of novel vascular health markers.