COVID-19 and its variants:
How N95 (hi-fi) masks can protect us
One of the defining issues of the COVID-19 pandemic and efforts to prevent its spread is inter-household transmission. Among the many policies and guidelines implemented, masks have been one of the most important and are now required wearing in the public spaces of many countries. But what if the masks we currently wear aren’t good enough? Researcher Devabhaktuni Srikrishna models the use of masks in different indoor scenarios. His MedRxiv preprint explores how N95 masks (FFP2 in Europe) or masks with high-fit/filtration (hi-fi) could be significantly more effective at preventing the inter-household spread of COVID-19. These masks could save lives, and if used consistently by a sufficiently large majority of people (in conjunction with sensible hygiene) could help to control the pandemic within several weeks.
What was once an unfamiliar sight has now become part of everyday life: face masks. The onset of the pandemic in late 2019 was a scenario the public health community had feared for decades. The newly discovered coronavirus (COVID-19) spread rapidly around the world. With COVID-19 cases still very much a part of our daily life and with new, more contagious variants emerging, it’s important that we use the right interventions and know-how to keep others, and ourselves, safe.
Evidence shows that, when used correctly, face coverings may help prevent us from passing the coronavirus to others. The WHO recommends that “masks should be used as part of a comprehensive strategy of measures to suppress transmission and save lives.”
When someone coughs or sneezes, breathes or speaks, sings or screams, particles containing water are released into the air. These particles may carry biological matter such as viruses if they are infected. Face masks and coverings work by preventing these particles from spreading and infecting other people. Since many people don’t develop symptoms, it’s possible to have the virus without knowing it and pass it to others.

Masking over the pandemic
Stopping the spread between different households (inter-household spread) has been one of the pivotal strategies of public health policy for tackling COVID-19. Inter-household spread is far easier to control, as these interactions are shorter and easier to avoid than intra-household spreading (within the home). Inter-household interactions – whether at schools, shops, or other businesses – are the foundation of a pandemic; the potential range and variety of people one can be exposed to outside of one’s home is self-evident.
Stopping the spread between different households (inter-household spread) has been one of the pivotal public health strategies for tackling COVID-19.
There have been many laws and guidelines implemented in the last year to prevent the inter-household spread of coronavirus. Outside of the most severe lockdown measures, none has captured our attention quite like masks. Visually, they are possibly the most distinct signifier of our pandemic world. However, there may be limitations with the masks we use. As the disposable N95 masks (FFP2 in Europe) are considered the most effective type of mask, they have been earmarked for healthcare or frontline workers. This has meant that many people have bought cloth masks.
Cloth masks are widely available and easily accessible, and are a cheaper option due to their reuse value. But that comes with a caveat – they aren’t as effective at filtering out aerosols (airborne viral particles) as their N95 counterparts. These are N95 masks which the US Centers for Disease Control and Prevention (CDC) have confirmed can filter at least 95% of airborne viral particles. N95’s axiomatic 95% filtration rate trumps the comparatively meagre 30% or less filtration efficiency measured in many cloth masks. Indeed, if everyone consistently wore reusable or disposable N95 masks when interacting (sharing the air) with people outside their household or bubble, the pandemic might well already be behind us.

N95 masks
Manufacturers report that N95 masks and other masks with similarly high filtration and fit (hi-fi) are no longer in short supply. Reusable masks with N95 or better protection called elastomeric masks (eN95) are in widespread use and have approval from the NIOSH, the CDC division that specializes in preventative measures in public areas. Use of elastomeric masks could be well timed for Spring 2021, when some public health experts warn that there could be another spike of COVID-19 cases due to variants. Only with effective public health protection can we protect ourselves and each other to help slow the spread of the pandemic.
Researcher Devabhaktuni Srikrishna modelled viral transmission in three different types of rooms. In the study, within each room, three different mask-wearing scenarios were compared: cloth masks, reusable N95 masks, and no mask wearing. Srikrishna looked at a standard room of six people, a bar of 18, and a classroom of 26 people. The three rooms were chosen as they packed people into areas with small dimensions and poor air ventilation. In each scenario, one ‘Patient Zero’ was sitting with their unsuspecting friends, exhaling 60 infectious doses per hour over a four-hour period.
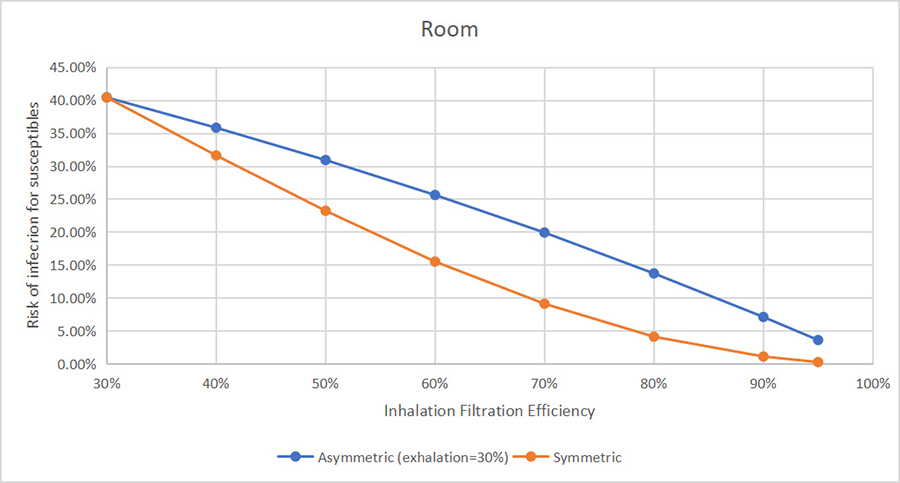


In the classroom scenario without masks, Srikrishna’s modelling predicted nine cases would arise within four hours. This is already disconcerting, particularly as many non-high schools can’t enforce that students wear masks. But the more disturbing finding was that that five out of 26 people were infected even wearing cloth masks. The only safe course of action was N95 filtration masks, which model near zero transmission risk in all three scenarios. In the classroom and bar scenarios modelled, there was only a 1.5% chance of infection when people wore N95 masks with a valve (accounting for 95% filtration upon inhalation and reduced 30% filtration upon exhalation, using a cloth-equivalent cover over the valve).


Srikrishna notes that the modelling makes several assumptions about contagiousness of viral emissions in exhaled breath, accumulation of aerosols, and filtration. These can vary in real life from situation to situation and are explained in detail in the MedRxiv preprint. He cautions these results are illustrative and should not be extrapolated to any individual situation without conducting site-specific and scenario-specific modelling.
In the scenarios modelled, there was only a 1.5% chance of infection when people wore N95 masks.
The data modelled by Srikrishna shows that hi-fi masks can help to provide an alternative to the never-ending cycle of lockdowns and exponential death spirals. In conjunction with other public health control measures (i.e. vaccines, testing, etc.) not only will masks save lives, but can help to prevent the social and economic damage necessitated by lockdown, keeping schools and businesses open.

Click here to view the image in a separate window
Q&A Section
Research Outreach spoke to Sri at his home office in California, to learn more about his work and find out how to put his findings into practical use.
Hi Sri! What makes the N95 mask (FFP2 in Europe) so effective?
Five key qualities have been identified as important for mask quality. These are high filtration, superior fit, durability, breathability, and quality control. Filtration is the ability to remove the virus-containing particles (around 0.1μm – 10μm size) from the air we breathe. Most high-filtration masks use electrostatic charges to capture these small particles (think of how small socks get stuck to larger clothes in a dryer – that’s due to electrostatic charges). For the N95 (FFP2) mask, the filtration exceeds 95%. Some masks are higher still, with up to 99% filtration or more. But all these factors are built into the N95-standard – they’re critical for us to protect ourselves and are not part of typical cloth masks for instance.
There are many different masks available that are great alternatives to the N95. These meet the five qualities listed above. They include the elastomeric N95 (eN95) and other hi-fi masks. A good alternative is a surgical mask (3-ply electrostatic) that can be secured to the face with a good fitter. This can be a hi-fi mask.
You’ve spoken before about how important it is that a mask should fit correctly. Could you tell us more?
This is super important! Even if you’re wearing a high-filtration mask, if it doesn’t fit your face, it’s not going to work effectively. The best masks have a very solid, tight seal so that air doesn’t leak. A poor-fitting mask means poor filtration no matter how good the filter is. The elastomeric masks have been designed for superior fit. In one study involving 60 participants by the Australian Society of Anesthesiologists, 98% of elastomerics passed fit testing versus 57% of disposables. This suggests that (in general) it’s easier for end-users to form a face seal with an elastomeric than a disposable. The Airgami mask has a folded design based on origami principles. This helps achieve a tighter fit to the face. We’ve tried out many different masks and a shortlist of N95 masks and high-filtration (hi-fi) mask alternatives is available on our website, patientknowhow.com.
I hear that some masks have exhalation valves and if so how can they be used to protect others?
To protect others, many elastomeric (eN95) and disposable masks also need to be used with a workaround such as a secondary face covering (e.g. surgical mask) to filter the air from the exhalation valve. Although the CDC recently studied the maximum particle emissions through the valve and found they are close to or better than surgical masks or unregulated face coverings. Some manufacturers address this by completely plugging the valve (e.g. Envomask and MSA). This provides equal (95%) filtration in both directions.
Many people are bewildered by the large choice of masks, and there’s a lot of uncertainty over which are the most effective. What advice can you offer?
It is bewildering. I want to shine a light on this to help people benefit from the right mask. The first thing I’d look for is whether it’s N95 (FFP2) standard. Go for a mask with similar properties. Take a look at our website, patientknowhow.com.
There’s an assumption that N95 masks or hi-fi masks are more expensive than many other products. Is this correct?
Prices of disposable N95 masks vary and typically cost US $2-5 each. They last between single-use to several days, depending on the duration and environment they’re used in (e.g. healthcare versus grocery store). There are good low budget options, e.g. the surgical masks (3-ply with electrostatic material) – many have 90-95% filtration built into the material depending on the manufacturer. If you then add a fitter on top, you have an even better mask. There are great, low-cost solutions for as low as $1 in the US, such as KF94 masks. These masks hug your face giving a great fit. Elastomerics (eN95) such as the 3M are very durable and can last up to one year as long as the filter cartridges remain in good condition. So although the initial cost is higher ($20-$80 depending on model), eN95 can be more economical in the long-run. This is perhaps the most important piece of clothing that we can wear right now. Hi-fi masks are cheaper than a pair of shoes. It’s a question of making it a priority.
There are some exceptions for mask wearing for individuals with health complications, such as breathing problems for example. Will N95 masks potentially create additional breathing related problems?
I’d always suggest that anyone with breathing difficulties or other health conditions should consult a doctor for advice on the right mask for them. But there are lots of off-the-shelf products, like the 3M elastomeric mask with P95 filter that has decent breathability. For example, two new designs (Airgami and Canopy) both report great breathability in testing due to the large surface area of their filters. I’ve been cycling in my elastomeric masks. There are lots of different options available to suit us all.
What difference would it make to the pandemic if we all wore effective, hi-fi masks?
If we wear hi-fi masks correctly when we‘re exposed to others (outside our household bubble), and if we maintain sensible hand hygiene then there are fewer pathways for the virus to transmit. By wearing hi-fi masks we may literally stop the spread of the virus in its tracks. I believe we could slow the pandemic in a matter of a few weeks. Senior citizens and those at higher risk from COVID have been offered free FFP2 masks in Austria and Germany. I think we should all follow their example. It’s an easy way to protect people. To me, it’s a no brainer. Get the right solution into everyone’s hands!
Could you tell us more about your previous work on public health strategies for other pandemics including Ebola and Zika?
I started out by building municipal Wi-Fi mesh networking devices. On the back of this, in 2014 I was involved in the Ebola response in Guinea during the West African Ebola epidemic. That work is directly responsible for me working on masks now. Being in the middle of infectious disease control like that made me realise how vulnerable we are. I’ve done research on ‘flattening the curve’ of novel viruses including Ebola, Zika, and now on Coronavirus. I strongly feel that with masks the solution for the Coronavirus pandemic is available to us. I hope we can shift the thinking around this and give people alternatives.