Inflammatory bowel disease and epithelial barrier function
Inflammatory bowel disease (IBD) occurs when the epithelial cells lining the gut become weakened, allowing gut microbes to activate immune cells. Gut barrier weakening can be caused by a loss of function of the PTPN2 gene. Professor Declan McCole of the University of California, Riverside and various collaborators have extensively researched the role of the epithelial barrier in IBD, the role of the PTPN2 gene, and potential targets for future treatment of this disease. The McCole group has also demonstrated that low gravity environments such as outer space have a negative and long-lasting effect on the epithelial barrier.
The cells that line the insides of human intestines (epithelial cells) have an essential role to play in forming a barrier against any possible infectious agents that could be present in food material, as well as helping to break down food into nutrients that can be absorbed, and taking up water to prevent dehydration. They provide a separative layer between the contents of the intestine and the underlying tissue and vasculature. Crohn’s disease and ulcerative colitis are both chronic inflammatory conditions of the human intestine and are collectively known as inflammatory bowel disease (IBD), which affects millions of people globally. An early change in IBD is reduced function of the intestinal epithelial barrier, which allows gut bacteria to access intestinal immune cells and causes a cycle of inflammation, further weakening the intestinal barrier. This increase in intestinal permeability is commonly referred to as leaky gut syndrome.
The causes of IBD are not fully understood, but genetics and changes in the natural gut microbiome (the population of microorganisms such as bacteria) are known to be critically important. The intestinal epithelial cells form a barrier of selective permeability which protects from invasion by the normal bacteria present in the gut. When the barrier is compromised, bacteria and their products can attack the cells and cause inflammation, which can (in severe cases) cause sepsis. Professor McCole has focused his research on these barrier cells and their role in chronic inflammatory gut conditions. The McCole group has also collaborated on studies into therapeutic avenues for IBD and the effect of low gravity environments on intestinal epithelial cells.

PTPN2
The protein tyrosine phosphatase non-receptor type 2 (PTPN2) gene produces the T-cell protein tyrosine phosphatase (TCPTP). This protein is essential for regulation of inflammation. Loss of function of the PTPN2 gene is associated with several autoimmune diseases including Crohn’s disease, ulcerative colitis, coeliac disease, type 1 diabetes and rheumatoid arthritis. The PTPN2 gene is therefore an important susceptibility marker for IBD and other diseases of the immune system.
Understanding the relationship between loss of PTPN2 function and IBD can highlight areas for intervention to help to reduce symptoms.
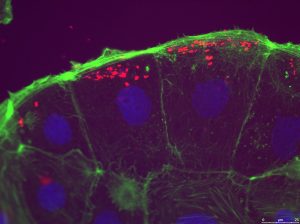
In 2009, the McCole group were the first to identify that absent function of this gene weakens the epithelial cell barrier. They have since built on this observation, alongside Dr Marianne Spalinger, Dr Meera Nair and Dr Michael Scharl, to demonstrate that PTPN2 controls the interactions between macrophages (immune cells that eat bacteria and viruses) and intestinal epithelial cells to maintain the epithelial barrier and therefore a healthy intestine. It was also shown that a loss of the PTPN2 gene promotes a more inflammatory gut environment. Mice with an absence of the PTPN2 gene have been demonstrated to have both increased levels of inflammatory cytokines (substances produced by cells which promote inflammatory responses in other cells) and uncontrolled inflammation. The disruption of the communication between intestinal epithelial cells and macrophages affects both the immune response and the integrity of the intestinal barrier. This research gives new insight into the role of genetic susceptibility in gut barrier function and therefore in IBD (1).

Clinical applications
Modulation of inflammation by TCPTP is partly via control of inflammatory signalling pathways, namely by inhibiting Janus kinase (JAK) enzymes and signal transducer and activator of transcription (STAT) molecules. JAK-STAT signalling pathways can be activated by inflammatory cytokines such as interferon-gamma, which is associated with autoimmune diseases including IBD and coeliac disease.
Understanding the relationship between loss of PTPN2 function and IBD can highlight areas for intervention to help to reduce symptoms, for example by targeting the pathway between loss of function in PTPN2, epithelial barrier regulation and the immune cells for personalised treatment of IBD. Studies by the McCole group have shown that one specific probiotic bacterial formulation (which is approved for clinical treatment of IBD patients following a specific type of surgery) increased the activity of the PTPN2 gene and therefore improved the function of the epithelial barrier (2).
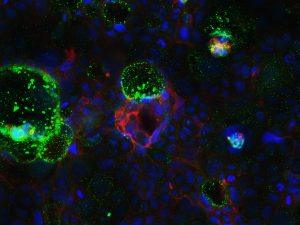
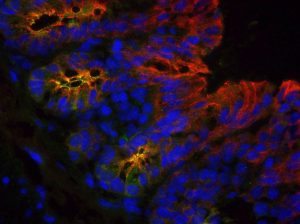
One recent study, in which the McCole group collaborated with Dr Adrian G. Butt, showed promising results for epithelial barrier maintenance in IBD patients treated with tofacitinib (the main component of the drug Xeljanz). Tofacitinib is a JAK inhibitor, and therefore blocks the activity of JAK enzymes involved in the inflammation causing IBD. In this study, stem cells were used to grow artificial human intestinal epithelial structures, which were then exposed to interferon-gamma, an inflammatory cytokine associated with IBD. It was shown that tofacitinib could actually restore the integrity of the damaged epithelial barrier. This was the first study to highlight the importance of the gut epithelial cells as a therapeutic target of tofacitinib (3).
The gut microbiome
Changes to the normal gut microbiome are an important factor in the disease process of IBD. Environments which allow expansion of intestinal bacteria that have the potential to attack the epithelial barrier contribute to the development and progression of IBD. In collaboration with microbiologists Dr James Borneman and Dr Ansel Hsiao, The McCole group investigated the relationship between PTPN2 and adherent-invasive E. coli (AIEC). AIEC is a specific type of E. coli bacteria which is known to colonise the intestines of sufferers of IBD, and is thought to be involved in the disease process as it increases the production of inflammatory cytokines as well as altering the regulation of the proteins forming junctions between epithelial cells (4).
Changes to the normal gut microbiome are an important factor in the disease process of IBD.
Mice lacking the PTPN2 gene showed a greater population of a novel mouse AIEC when compared to mice with a functional PTPN2 gene. This mouse AIEC showed similar properties to the AIEC associated with IBD in humans. This mouse AIEC was shown to not only increase the severity of colitis in mice, but also to prevent recovery from it. This study therefore demonstrated that the PTPN2 gene regulates the normal gut microbiome to protect against novel infectious agents; and consequently, loss of function of the PTPN2 gene contributes to an altered gut microbiome which allows the proliferation of an AIEC which can both initiate and worsen disease. Future research could build on these findings by using PTPN2-deficient mice as a model to study the relationship between host genetics and the gut microbiome. These studies have enabled the McCole group to build a more interconnected view of the delicate balance between the epithelial cells and the gut microbiome and how disruption of this balance can contribute to diseases such as IBD.
Microgravity
Professor McCole’s group, together with Dr Kim Prisk, investigated the previously little-understood effects of microgravity (low gravity environments, as would be experienced in outer space) on the epithelial cell barrier (5). Previous studies in the field of space biology have demonstrated that microgravity can have a negative impact on the human immune system, via suppression of multiple immune cells. This study aimed to assess the permeability of the epithelial barrier cells and their susceptibility to infection in microgravity environments. Using a rotating bioreactor to create an environment of controlled loss of gravity, epithelial cells were placed in simulated microgravity and then assessed for permeability. Simulated microgravity was shown to cause disruption to the epithelial barrier. This reduced function was demonstrated to continue after returning to a normal gravity environment, increasing their potential susceptibility to invasion of the epithelial cell barrier. This has long-term implications for the gut health of individuals undertaking missions into outer space. Understanding the effects of low gravity environments on the human body can allow organisations such as NASA to better prepare and protect their astronauts.
Conclusion
Epithelial cells play a critical role in maintaining a barrier between the intestinal contents and the body’s tissues, and disruption to this barrier can cause an ongoing cycle of inflammation. The barrier may be compromised by chronic disease such as IBD or by abnormal environments such as microgravity. Understanding the effect of genetics and environment on the epithelial cell barrier allows potential therapeutic areas to be targeted to relieve sufferers of symptoms of both acute and chronic intestinal disease.
Personal Response
What are the next steps for your research?
<> Our ongoing work is investigating more detailed molecular mechanisms by which loss of PTPN2 activity in mice and IBD patients genotyped for loss-of-function mutations, leads to disruption of key cellular structures (tight junctions) that govern permeability between epithelial cells. Tight junctions represent a critical target in conditions that weaken the intestinal barrier as they can be reorganised by inflammatory cytokines and bacteria with pathogenic properties. Additional studies will determine if JAK inhibitors can be used to correct underlying gut barrier defects in mice lacking PTPN2. This could improve targeting of JAK inhibitors to treat specific patients. New NIH funding will allow us to determine additional mechanisms by which epithelial cells and intestinal immune cells (macrophages) act cooperatively to protect barrier function.