Rib fracture pain and disability: Do we need a more aggressive approach after all?
Rib fractures are the most common injury after thoracic (chest) trauma, accounting for approximately two-thirds of cases. The main challenge in treating them is controlling the associated pain that can lead to complications, such as chest infections and respiratory failure. Despite advances in pain control and anaesthesia, the conservative treatment of these injuries often results in chronic pain, in some cases lasting up to two years after the injury. Dr Benoît Bédat and his team at the University Hospital of Geneva in Switzerland, are currently investigating rib surgery as a more efficient way of treating rib fractures.
Rib fractures are quite common after blunt trauma to the trunk, with motor vehicle crashes and falls being the leading causes. In some cases, they can result in complications such as pneumothorax or haemothorax, occurring when air or blood leaks into the chest cavity, occasionally compressing the lung and leading to respiratory failure unless urgently treated.
In the majority of cases, rib fractures are uncomplicated. However, because of the associated pain, patients with such injuries often need to be admitted to hospital for pain control. They are usually treated with oral analgesics, including narcotics and nonsteroidal anti-inflammatory drugs, and, in the case of persistent and intense pain, patients have to be given epidural analgesia or rib blocks.
In most trauma centres and hospitals, rib fixation surgery is reserved for patients with unstable rib fractures or flail chests – occurring when a segment of the rib cage is ‘floating’ as a result of two or more consecutive ribs fractured in more than two places each.

Conservative treatment is not always enough
A common dogma among doctors is that pain after rib fractures that have been treated just with pain relief lasts up to six weeks. Unfortunately, this isn’t really the case. There are recent studies describing persistent pain and disability, with up to 76% of patients with uncomplicated rib fractures reporting pain at two months after the injury, and up to 56% of them still complaining of pain six months after the injury. Approximately 13% of patients report that their quality of life is being affected by chronic pain one year after simple rib fractures. Additionally, in another study, 30% of patients with rib fractures that had been managed conservatively with standard pain relief were not able to return to pre-injury employment even two years after their injury. This significant long-term pain and disability has a huge socio-economic impact and is putting increasing pressure on doctors to find and try alternative treatments for uncomplicated rib fracture injuries.
30% of patients with rib fractures that had been managed conservatively were not able to return to pre-injury employment even two years after their injury.
Is there an alternative?
A recent American multicentre, prospective, controlled clinical trial revealed that there might be an answer in costal-fixation surgery for uncomplicated rib fractures, especially since it showed an improvement in pain-intensity levels within the operative group, as compared with the non-operative group. It also showed an improvement in the same group regarding co-morbidities and opioid analgesic consumption. Similarly, an Australian study investigating the quality of life after rib fractures suggests that patients who underwent rib osteosynthesis (rib-fixation surgery) had less post-operative pain and also less long-term pain and disability issues.
Since the only predictive factor for ongoing pain and disability identified so far is the pain intensity during the first few days after injury, it has been suggested that the possible mechanism leading to the chronicity of the pain after rib fractures is that the initial high-intensity pain might be sensitising the central nervous system to pain perception. Therefore, an early interventional approach to reduce acute pain after rib fractures might improve the outcomes for these patients.

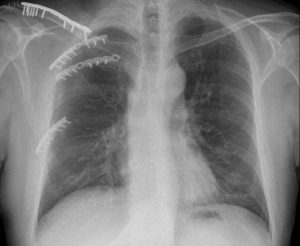
X-rays of a rib fracture: left) Before rib osteosynthesis, right) After rib osteosynthesis.
The PAROS study
Dr Benoît Bédat is the principal investigator for the PAROS (Pain After Rib OSteosynthesis) study, a multicentre randomised clinical trial that aims to compare the pain-control effect of rib-fixation surgery to that achieved with just standard medical analgesia in patients with uncomplicated rib fractures. The team’s hypothesis is that costal surgery, on top of the standard analgesia, may further control the pain related to rib fractures. The rationale behind this hypothesis is that costal fixation could lead to reduced inflammation and nerve injury by restricting and preventing further fracture movement and thus reducing pain.
Since there is no previous study that provides enough evidence to recommend rib fixation as a treatment for uncomplicated rib fractures, the aim of the PAROS study is to investigate the benefits of surgery and the possibility of it becoming an approved treatment option in the future.
More specifically, the team is planning to compare the reduction of pain levels between a patient group that will undergo rib fixation and another one that will be treated with standard medical analgesia alone. The comparison is going to take place at baseline, one, two, three, six and 12 months after injury/surgery. It is of note that PAROS is the only trial so far looking at the long-term effectiveness of the two types of pain management (operative and non-operative) in comparison. The pain will be assessed using specific pain-scoring systems. Surgery is to be performed within five days from the injury, and the team will follow specific inclusion and exclusion criteria. The study will be performed in three tertiary-care hospitals in Switzerland.
An early interventional approach to reduce acute pain after rib fractures could potentially improve the outcomes for these
patients.
Secondary objectives of the study include comparing the amount of pain relief used by both teams, the length of the hospital stay, levels of anxiety and depression related to the injury in both groups, lung function after the injury, and finally, the productivity impairment between the two treatment groups against the direct costs of the treatments for the two groups respectively.

Surgical procedure and devices
The surgical procedure will include general anaesthesia, muscle-sparing thoracotomy – which is an incision on the chest wall – and rib-fixation surgery using special fixation devices to stabilise the chest wall.
The devices that will be used in the trial have already been in use in other trauma centres. They include different types of rib-fixation systems produced by a few different companies, including MatrixRIBTM, De Puy Synthes Companies®, Zuchwil, Switzerland, STRATOSTM, MedXpert® GmbH, Heitersheim, Germany, NITI Fixing PlatesTM, and IAWAl®, China. According to the team, every system can be used for all patients and for all rib fractures.

Leah-Anne Thompson/Shutterstock.com
Conclusion
Rib fractures are a very common injury often associated with immense levels of persistent pain and disability, which have a large psycho-socio-economic impact on patients and our healthcare systems. Although there are many challenges when it comes to the treatment of rib fractures, including the lack of clinical research and evidence, it is quite obvious that the current conservative treatment of rib fractures does not efficiently facilitate pain relief or even a prompt return to everyday activities. New methods for treating rib-fracture patients that alleviate pain and reduce disability are urgently required and are expected to have a positive impact – not only on individual patients but also on the wider community.
It therefore doesn’t come as a surprise that the surgical treatment of rib fractures in the absence of a flail chest is drawing increased surgical attention lately. Dr Bédat and his colleagues are planning to put the surgical intervention under the microscope and evaluate it as a possible standard treatment of care for patients with non-complicated rib fractures.

Personal Response
Do you think that there is a place for Video-Assisted Thoracoscopic Surgery (VATS) in the near future of rib fixation surgery?
Thank you for your question. There are several limitations to the use of VATS in rib fixation. Rib fixation requires sufficient space for the surgeons to have good access to the fractured rib in order to be able to fix the plate on the rib on both sides of the fracture, especially when the case is difficult. VATS is an endoscopic (keyhole) procedure and that means the exposure it provides, and therefore the space available for the surgical interventions, is quite limited. Additionally, VATS is a procedure that requires direct contact of the surgical instruments with the lung, something that – besides the technical difficulties that it poses – could also lead to pulmonary or infectious complications.